One app oversees the anesthesia machines throughout the hospital, tracking daily equipment checks, to help ensure that the right machine is ready for the right patient at the right time. When Mulier starts to administer anesthetic gas, another app monitors the gas flow rate. Another tracks and measures how the patient’s delicate lungs are faring during surgery. In the near future when Mulier dials back on the gas, another app will notify a nearby nurse so she can ready a recovery room or perhaps prep the next OR patient.
“These apps help us follow the guidelines to avoid troubles and complications,” Mulier says. “We’re now seeing fewer patients with atelectasis (lung tissue collapse) post-operatively with better oxygenation and fewer pulmonary complications.”
The apps, which Mulier has been using for the past few years, are all part of GE’s Carestation Insights, a suite of applications that run in conjunction with GE’s Aisys CS2, a fully digital anesthesia machine, to crunch massive amounts of data.
To be sure, the apps act only in an informative role. They don’t control the anesthesia process. That’s the doctor’s job. But combined, the digital machine and its accompanying apps help clinicians deliver the right levels of anesthetic gas for their patients.
 “These apps help us follow the guidelines to avoid troubles and complications,” says Dr. Mulier. Image credit: GE Healthcare.
“These apps help us follow the guidelines to avoid troubles and complications,” says Dr. Mulier. Image credit: GE Healthcare.Of the suite of apps, the one that is an immediate asset to patient care is the Lung Protective Ventilation app. The process of administering anesthesia can be hard on the patient’s lungs, as patients must remain on a ventilator with the sleeping agents pumped into their airways. Incorrect mechanical ventilation — supplying too much gas with every single breath, for example — can cause trauma to the lungs and lead to inflammation that can later spread through the body, possibly leading to sepsis.
The Lung Protective Ventilation app is designed to help doctors shine new light on the problem. The app presents anonymized patient and device data from past procedures, such as the air pressure that remains in the lungs after exhalation — doctors call it PEEP, for positive end-expiratory pressure — and lung compliance, which measures how stiff the lung is. The idea is that the insights from past cases can help doctors adjust ventilation to achieve the best outcomes in the future.
“Guidelines for lung protective ventilation are easy to understand,” says Mulier, who added the Ventilation app to his roster last year. “We do not need difficult measurements, calculation or interpretation to find what to do. We need simple methods, running in the background without any extra work, to verify that we are following the guidelines. This is not to blame people but to stimulate them to improve their practice by showing each one his or her results.”
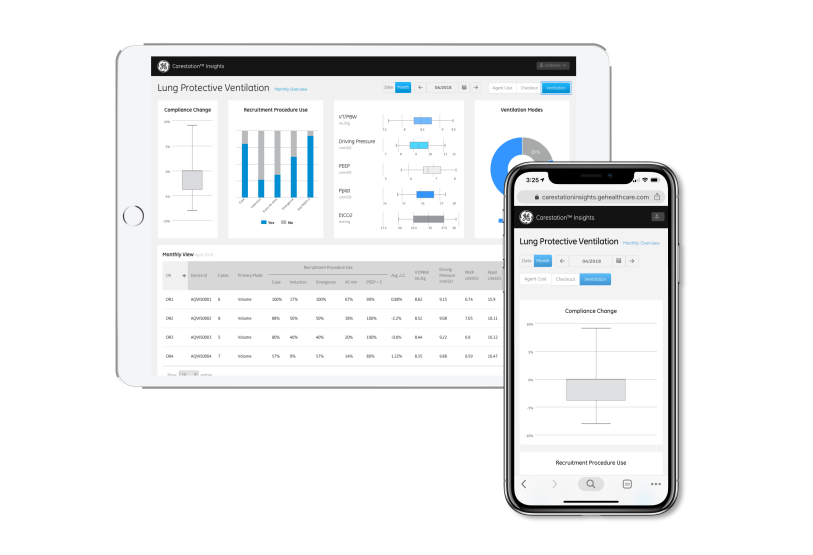 GE’s Carestation Insights is a suite of applications that run in conjunction with GE’s Aisys CS2, a fully digital anesthesia machine, to crunch massive amounts of data. Image credit: GE Healthcare.
GE’s Carestation Insights is a suite of applications that run in conjunction with GE’s Aisys CS2, a fully digital anesthesia machine, to crunch massive amounts of data. Image credit: GE Healthcare.The latest app on the Carestation Insights platform, OR Workflow, is focused more on logistics. It offers a digital dashboard that shows the status of each patient procedure currently in an operating room. When the app notices a patient procedure soon to finish, it automatically and anonymously bumps that OR to the top of the readout, so staff can quickly see which person, and which room, they’ll need to focus on next for moving and cleaning.
“In terms of OR efficiencies, there’s a lot of handoffs that happen,” says Jack Page, a global product manager at GE Healthcare. “You can imagine the delays that communication challenges can result in.”
Mulier says this app will also help the mood in operating rooms. “This could help avoid interrupting and annoying the surgeon by asking, 'Will you be ready in the next hour or minutes?’,” he says.
Carestation Insights apps, which are available on an annual subscription basis, are already in use in hospitals in Europe, Canada, South America, New Zealand, South Africa and the United States.
In Bruges, Mulier says these apps have made it much easier for him and his team to see the big picture. “[Prior to the apps] we were able to measure this for each individual case but the data wasn’t recorded,” he says. “We now have a dashboard overview with all cases together showing a percentage of doing it right and a percentage of how many patients did still have a problem.”