Scientists used gene therapy to regenerate damaged nerve fibers in the eye, formulated a way to 3D-print cartilage found in the knee and developed a blood test that indicates infection with antibiotic-resistant bacteria in less than one hour. This week’s coolest scientific achievements are written all over the body.
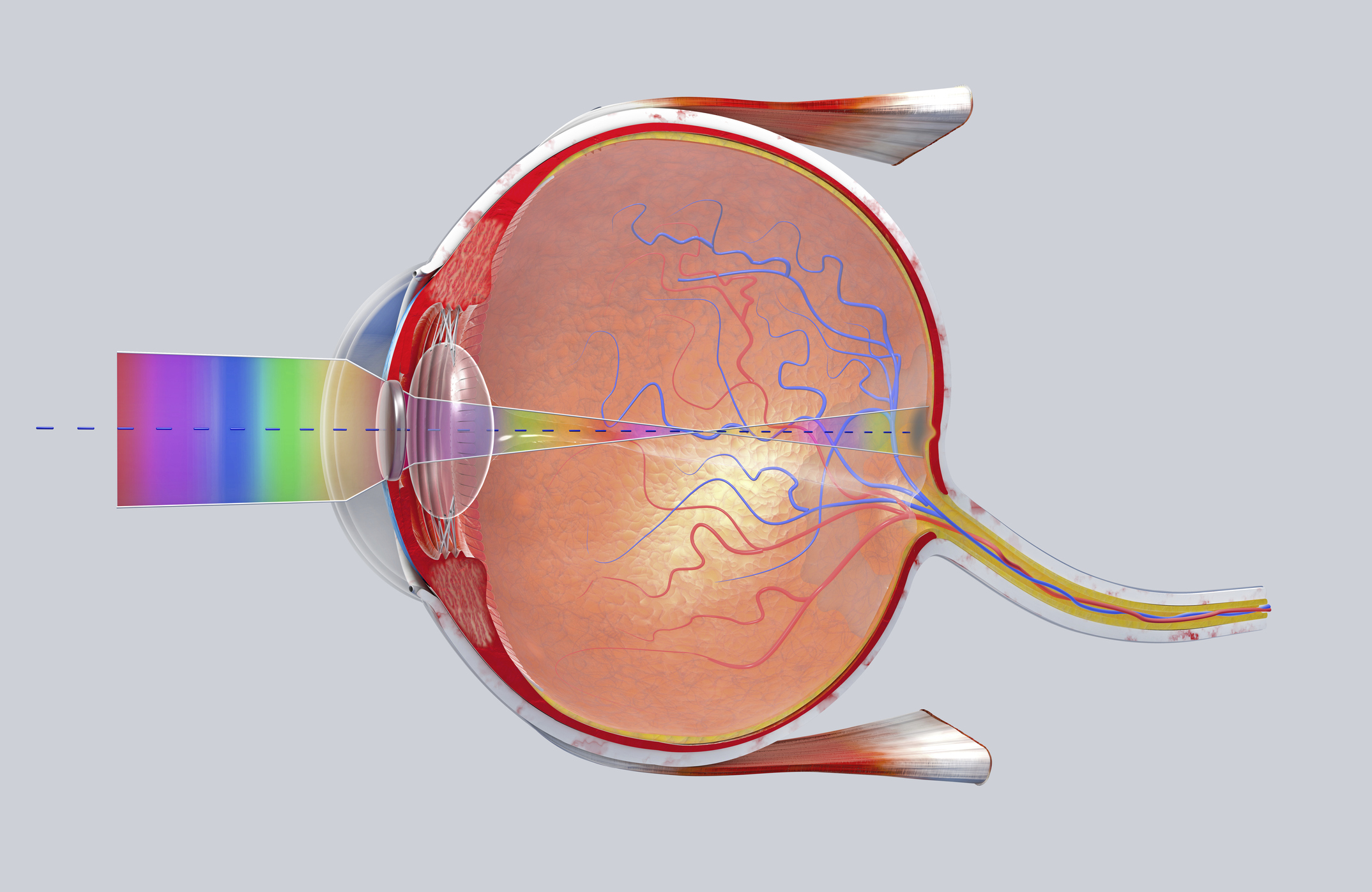
What is it? Researchers at the University of Cambridge used gene therapy to regenerate damaged nerve fibers in the eye, possibly pointing to a new way to treat glaucoma, which causes blindness.
Why does it matter? Glaucoma, which involves progressive damage to the optic nerve connecting the eyes to the brain, is “one of leading causes of blindness worldwide,” said Veselina Petrova, first author of a new study in Nature Communications. “The causes of glaucoma are not completely understood, but there is currently a large focus on identifying new treatments by preventing nerve cells in the retina from dying, as well as trying to repair vision loss through the regeneration of diseased axons through the optic nerve.”
How does it work? Those axons, or nerve fibers that carry signals to neurons, were the focus here. Typically, in the adult central nervous system, axons don’t regenerate after being damaged. In this study, though, scientists found that if they tweaked the gene responsible for the production of a protein called protrudin, the nerve cells increased their ability to regenerate. This study was conducted in vitro and Petrova said that it was “important to point out that these findings would need further research to see if they could be developed into effective treatments for humans.”
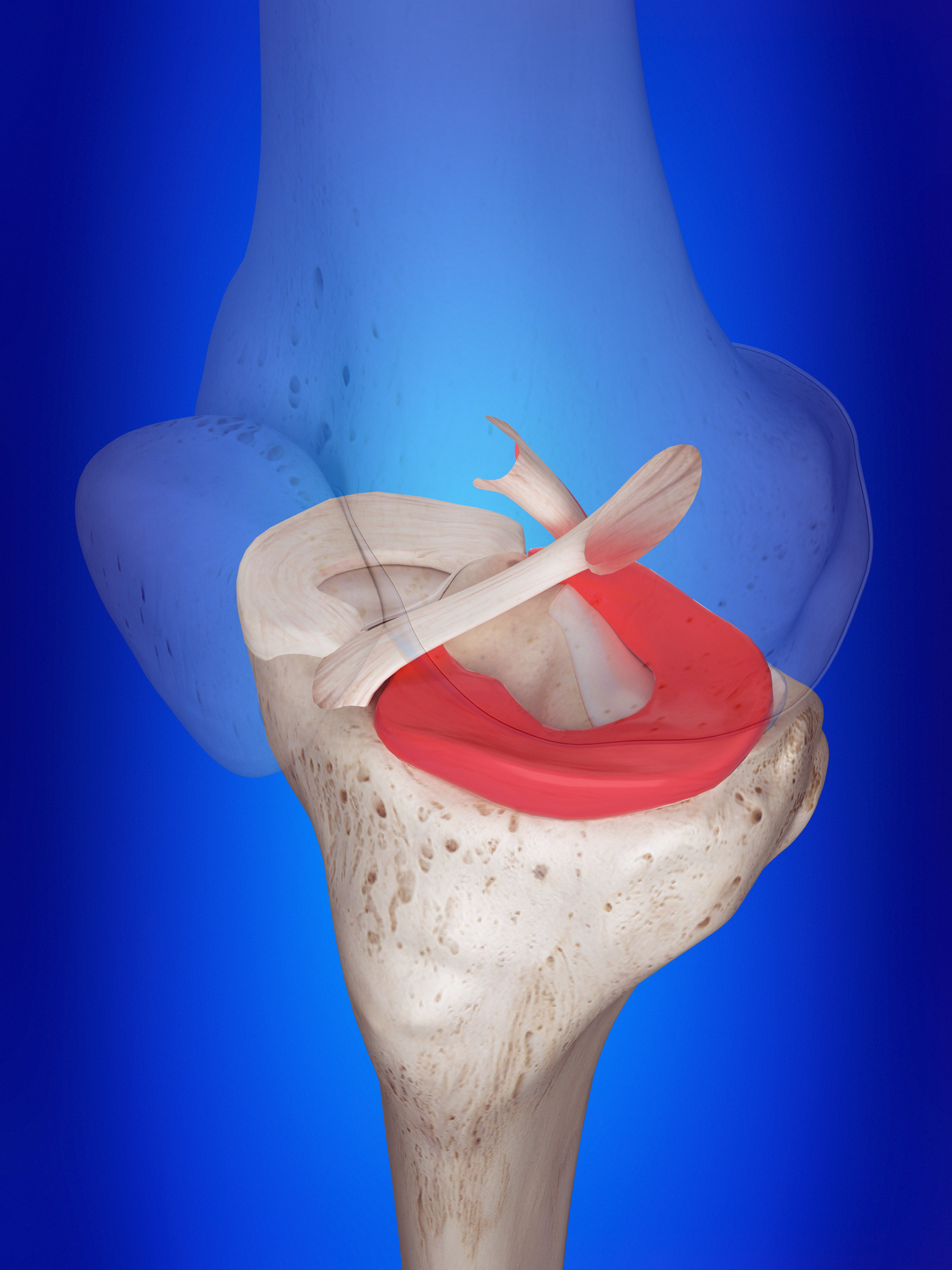
What is it? Researchers at the Wake Forest Institute of Regenerative Medicine developed a way to 3D-print a “hybrid tissue,” made of cells and hydrogels, that might someday help restore knee function for people with arthritis or injury.
Why does it matter? The type of cartilage that the hybrid tissue could replace is found in the meniscus, the knee’s “shock absorber,” and a site that’s especially susceptible to injury — as many athletes know. According to the Wake Forest Institute, “Degeneration of the meniscus tissue affects millions of patients and arthroscopic partial meniscectomy is one of the most common orthopedic operations performed.” There are few treatment options except surgery.
How does it work? Produced on a 3D bioprinter that itself took 14 years to develop, the replacement fibrocartilage is made of two special bio-inks and “provides a cell-friendly microenvironment and structural integrity.” As with all 3D printing, the machine lays down layer upon layer of the special inks into a new shape, which contains cells that could grow new tissues and organs. This study, published in Chemistry of Materials, was a proof-of-concept study, said Wake Forest Institute director Anthony Atala, that “helps point our work in the right direction to someday be able to engineer this crucial tissue that is so important for patients.”

What is it? An interdisciplinary team from Brigham Young University developed a test that can detect the presence of antibiotic-resistant bacteria in the blood in less than an hour.
Why does it matter? On a broad scale, antibiotic-resistant bacteria are a major health crisis. For patients, they’re a severe health threat that advances quickly in the body and can have lethal effects. Current testing methods can take up to 24 hours or longer, though, to return results. "Once you’re trying to diagnose the disease, the clock is ticking," said Aaron Hawkins, a professor of electrical and computer engineering and the co-author of a new study in the journal Lab on a Chip. “Every hour the disease is untreated, survivability drops by about 7%. You want to know what you’re fighting immediately so you can apply the right treatments.”
How does it work? As that journal name indicates, the method involves a chip. First researchers take a blood sample and spin it to isolate the bacteria, then DNA is extracted from the bacteria. The DNA is pushed through a fluid channel on a microchip, where a fluorescent signal will indicate the presence of antibiotic-resistant strains. Importantly, the chip can test for the presence of multiple resistant bacteria at once. The researchers plan to install the chip on a disposable, inexpensive cartridge that can be used in hospitals.
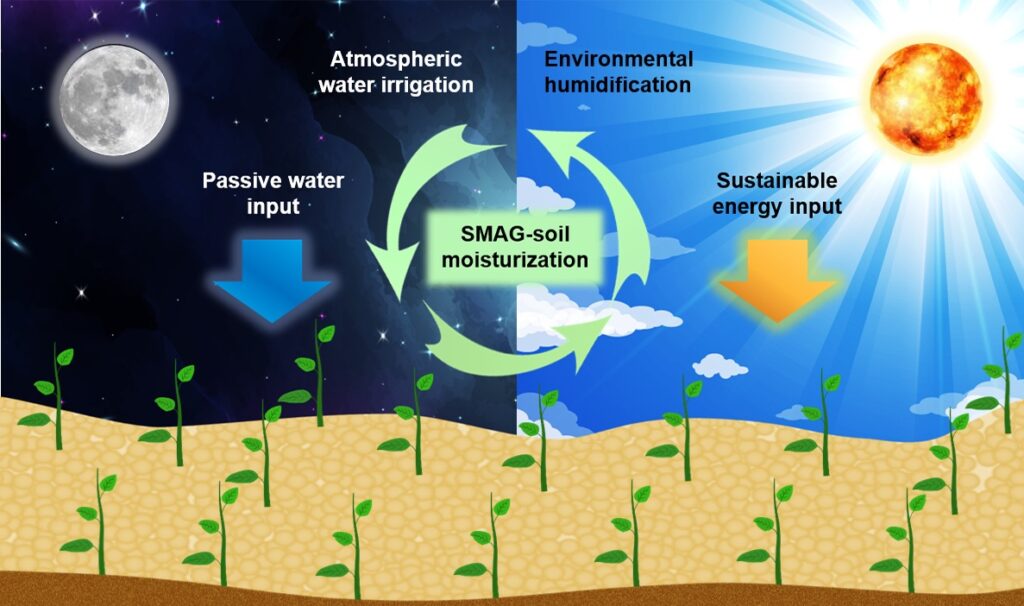
What is it? Engineers at the University of Texas at Austin created a new type of soil that can pull moisture from the air.
Why does it matter? The soil waters itself! But it’s not lazy gardeners it’s aimed at — it’s farmers in places where water itself might be scarce, and irrigation difficult. Guihua Yu, a professor of materials science and the co-author of a new paper in ACS Materials Letters, said, “Enabling free-standing agriculture in areas where it’s hard to build up irrigation and power systems is crucial to liberating crop farming from the complex water supply chain as resources become increasingly scarce.”
How does it work? The soil is made of gels that are super-absorbent. When the air is cool and humid — say, at night — the soil absorbs moisture, releasing it during the day when activated by warmer temperatures. In experiments in rooftop plots in Texas, Yu and team found that between 0.1 and 1 kilograms of the soil (depending on the crops) was sufficient to irrigate about a square meter of farmland. Farms might not be the only beneficiaries of this technology, though — researchers think it could be used to cool solar panels and data centers, and to expand access to drinking water.

What is it? Molly Shoichet, a chemical engineering professor at the University of Toronto, just won the Gerhard Herzberg Canada Gold Medal — the country’s top science prize — for her pioneering work in developing hydrogels that mimic human tissue.
Why does it matter? The 3D hydrogels have a range of potential applications. For instance, one of the companies created out of Shoichet’s work was recently approved to begin human trials on an anesthetic for post-surgery pain that involves an injectable hydrogel; Shoichet noted that pain resulting from surgery is one driver of the opioid crisis. “Everything that we do is motivated by answering a question in biology, using our engineering and chemistry tools to answer those questions,” she said.
How does it work? The broader significance of Shoichet’s work, though, relates to the ability to custom-design hydrogels to study specific problems — her lab has also used them to study drugs that could treat brain and lung cancer, as well as a rare lung disease. They allow cells to grow in a three-dimensional space just like they do in the body, which makes them useful, for instance, for drug development: “One of the challenges facing drug screening is that many of the drugs discovered work well in the lab, but not in people, and a possible explanation for this discrepancy is that these drugs are discovered in environments that do not reflect that of the body,” Shoichet said.





