The world’s doctors are now fighting against the COVID-19 pandemic on two fronts. The virus is still chiefly known as a lung-related affliction; its main symptom is a dry cough, which, in acute cases, can lead to viral pneumonia. But the new coronavirus also assails other vital organs, including the one that lies between the lungs: the heart.
The new threat means that hospitals don’t just need mechanical ventilators, which help patients to breathe, in their anti-virus arsenal. They will also rely on a pair of technologies that have been staples on medical wards for decades — electrocardiogram (ECG) and ultrasound. But this is not a story about hospitals falling back on two trusty warhorses. Today’s ECG and ultrasound machines sport state-of-the-art software that can keep close tabs on COVID-19’s assault on the heart, allowing clinicians to react early and save lives.
The versatility of the virus came as an unpleasant surprise. In March, researchers in China published a study of 416 patients hospitalized with the coronavirus showing that nearly one in five (19%) had sustained heart damage. That heart damage was particularly lethal; over half (51%) of these patients, whose median age was 64, later died. It may be no surprise to learn that patients in the study with pre-existing cardiovascular disease were particularly susceptible to a COVID-19-induced cardiac injury. But researchers found that a cardiac injury triggered by the new coronavirus could kill even those patients with no history of heart disease.
Doctors are still learning about the exact way that COVID-19 attacks the heart. One theory is that the virus infects the organ by glomming onto receptors in the muscle in the same way that it infects the lungs. “Think of a lock and a key — the keyhole has to accept the key,” explains Dr. Paul Friedman, who is chair of the department of cardiovascular medicine at Mayo Clinic. “The virus has a key called a spike protein, which binds to specific receptors in lung cells and heart cells.”
“There is strong evidence that patients suffering from COVID-19 are getting heart problems, whether it’s a direct effect of the infection or of a systemic infection,” says Kai-Uwe Lempertz, a global clinical development manager at GE Healthcare. He explains how viral pneumonia can “jump over” to the heart, causing myocarditis, or inflammation of the heart muscle.
The pathology of the virus as it relates to the heart may not be 100% clear, but there is no doubt about its effects. As well as myocarditis, several COVID-19 patients in the study developed an irregular heartbeat, also called an arrhythmia. Researchers have also reported that COVID-19 posed a particular threat to patients with existing hypertension, because the virus appeared to block the hormones that regulate blood pressure.
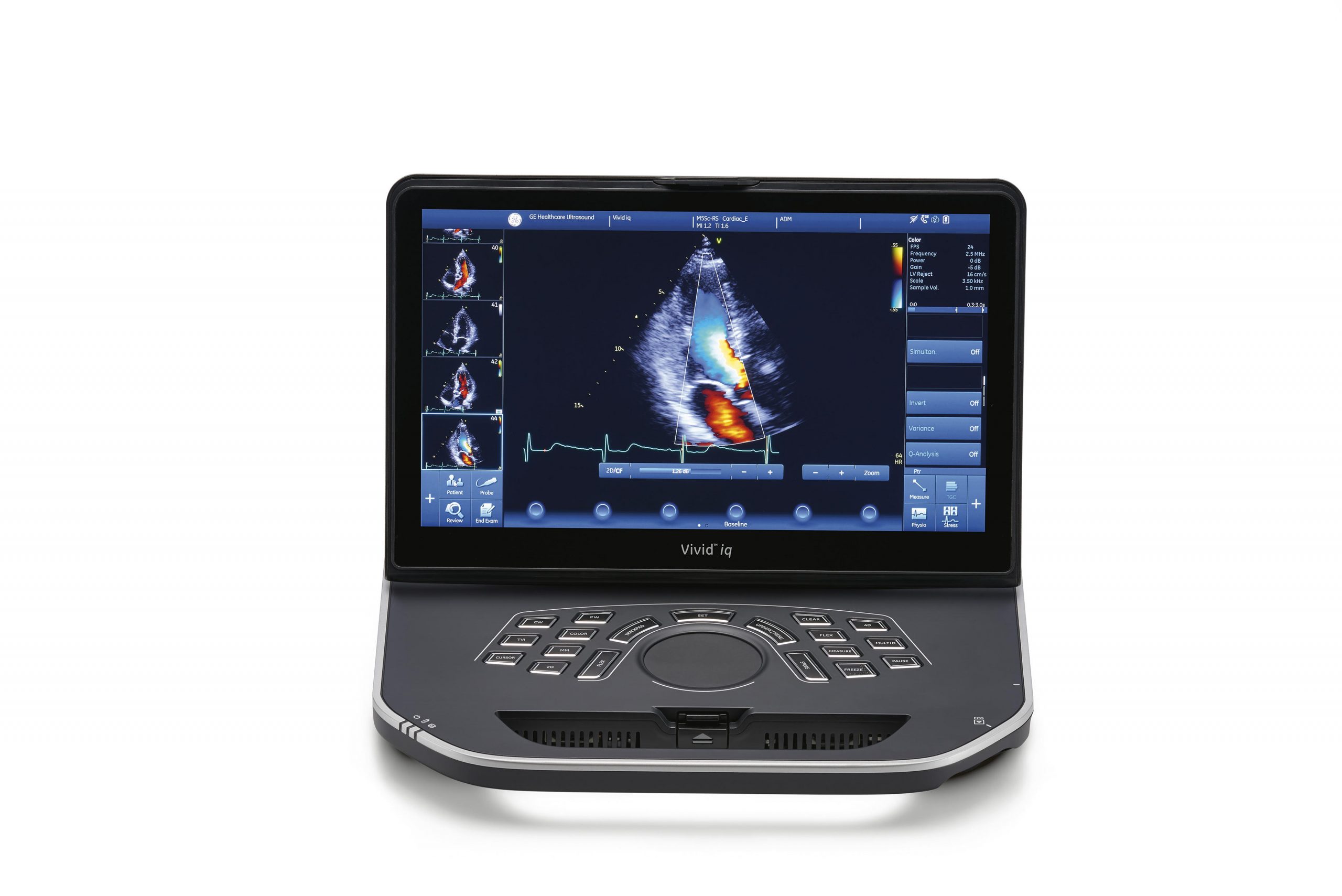
GE Healthcare's Vivid iq is a portable, battery-operated laptop-style ultrasound scanner with touch-screen functionality and a sealed surface for easy cleaning — an important consideration for reducing risk of infection. Top and above images credit: GE Healthcare.
“It appears to weaken the heart muscle in some way, which hampers blood flow, or it causes an electrical malfunction, which means that it doesn’t fire properly,” says Ashutosh Banerjee, global business head of diagnostic cardiology at GE Healthcare. He simplifies the situation with an analogy: The heart needs both a “plumber and an electrician” to keep blood flowing through its various veins, arteries and valves, and to ensure steady electrical impulses for contraction. The virus appears to block these two skilled tradespeople from doing their work.
Even though COVID-19 is a stealthy saboteur, it still leaves a distinctive trail, Banerjee adds: “It creates elevated biomarkers that we use to detect heart attacks.” Those biomarkers are like paw prints in the sand for clinicians who are tracking the virus. And this is where ECG and ultrasound machines come in.
Resting ECG carts are a staple of TV medical dramas: They’re the bedside devices that record the heart’s rhythm and electrical activity, emitting regular electronic blips and jagged waves. Tiny anomalies in the peaks and troughs of those waves can reveal that something isn’t quite right.
One of the key readings on an ECG is the QT interval, which is an indication of the time it takes a heart to recharge between beats. The prolongation of that QT interval, also referred to as “long QT,” is a concern for clinicians, because it sets the stage for an abnormal and potentially fatal heart rhythm called torsades de pointes, or TdP — French for “twisting of the points.”
“Instead of causing a normal coordinated contraction, the electrical signals become chaotic, they quiver, and the heart stops pumping and the person collapses,” says Friedman. “It’s not common, but it’s terribly important to know if someone’s at risk from that [TdP].”
There are no hard and fast rules, but experts generally regard a prolongation in excess of 500 milliseconds (ms) as risky. COVID-19 can lead to long QT but — in an added complication for clinicians — so can the treatment of the virus itself: Several standard medications including anti-arrhythmics, antibiotics and some anesthetics are also QT-prolonging drugs.
So are chloroquine and hydroxychloroquine, two drugs that have been discussed to have potential to treat coronavirus complications — but that are causing concern among scientists because of their possible impact on the heart. “They might be cardiotoxic for some patients, which increases the chances of sudden cardiac death,” explains Banerjee. If clinicians sense signs of trouble, they may need to urgently discontinue any QT-prolonging drug, adjust the patient’s electrolytes, administer magnesium sulfate or even consider a temporary pacemaker.
That’s why resting ECG machines have become important to clinicians treating COVID-19 patients. In particular, they’re using state-of-the-art 12-lead machines, so called because they monitor 12 different sites of the body, which helps to build up a detailed picture of the heart’s electrical activity, including QT intervals. After administering any drug, they can continue to monitor patients with the machines.
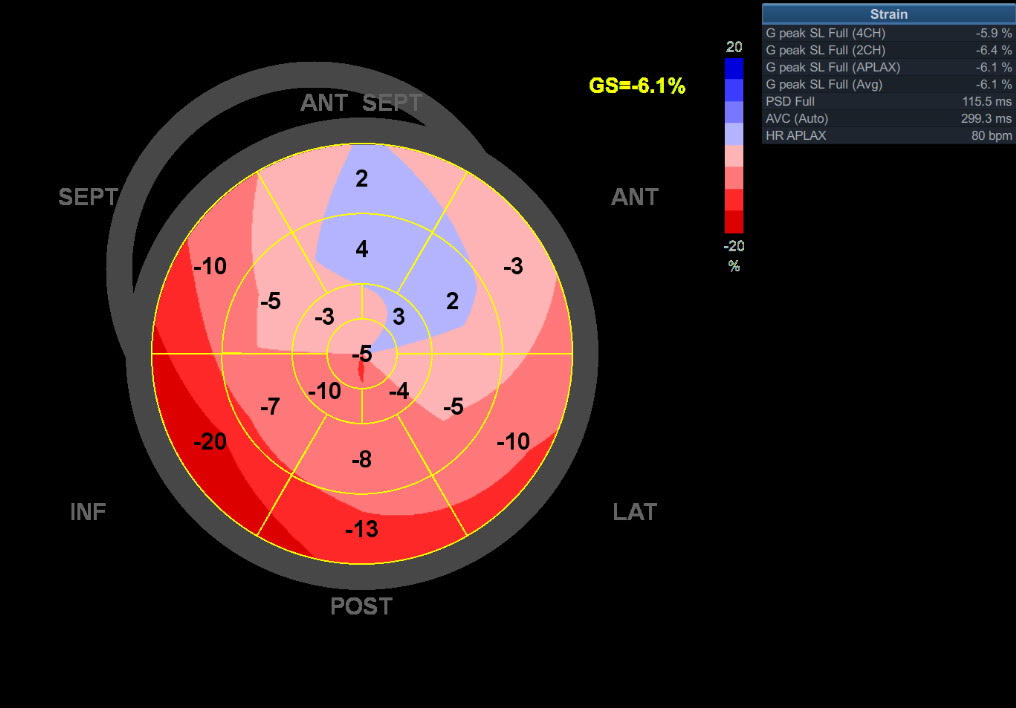
A malfunctioning left ventricle, quantified with the AI-supported Automated Function Imaging technology of GE Healthcare's Vivid iq. This technology is able to detect very subtle changes in the function of the ventricle. Image credit: GE Healthcare.
State-of-the-art machines such as GE Healthcare’s MAC VU360 Resting ECG can further help them monitor those cardiopulmonary complications. All of GE Healthcare’s diagnostic ECGs use a special algorithm that’s able to quickly deduce patterns in readings from an analysis of mountains of historical data, including an individual patient’s previous records. “It can tell in around 10 seconds whether a situation is good or bad,” says Banerjee. The algorithm can thus alert clinicians to emerging risks, such as lengthening QT intervals, which allows them to stave off a life-threatening TdP event.
Listening to the heart is vital — so is seeing it. Cardiovascular ultrasound can give doctors a clear image of the heart that allows them to detect abnormalities in the size and shape of the organ. For example, a cardiovascular ultrasound assessment will typically analyze the size of the heart’s left ventricle and its systolic function. That’s the name given to the phase of the heartbeat when the muscle contracts, and pumps blood from the chambers into the arteries. “It will tell you how efficiently the heart is pumping blood supply into the body,” explains Lempertz.
Imaging the left ventricle in this way allows the trained human eye to pick up on any abnormalities in its size and shape, says Lempertz. But artificial-intelligence-enhanced features on an ultrasound machine, such as GE Healthcare’s Vivid iq, afford a sharper image, enabling clinicians to measure the dimensions of the chamber and evaluate heart function.
There’s a bonus: Algorithms help clinicians to quickly acquire high-quality images with the laptop-sized machine before leaving the room, a process that takes minutes — important because it minimizes staff’s exposure to infection. “You can start it up in five seconds, get images and then get out,” says Lempertz. The machine can automatically send the images into a central image repository, which allows for remote analysis elsewhere in the hospital. “All the quantification can be safely done in a reading room, where people don’t need to wear protective equipment.”
The compact, ergonomic, easily adjustable design of the machines means they are well-suited for the intensive care unit (ICU), where many COVID-19 patients will be treated. Banerjee explains that the ECG carts are smaller and lighter than their peers, making them easier to maneuver. They also have the option of a 15-foot cable, which means that the cart doesn't even have to enter the ICU. “That might sound trivial, but it’s a big design feature that reduces the risk of infection, which protects technicians,” he says.
The ECG workstation also has smooth surfaces, making it easy to clean and disinfect. “We have compiled a list of many cleaning materials that kill COVID-19 and are compatible with our carts,” says Banerjee. The same goes for Vivid iq.
Unfortunately, expert clinicians suspect that virus survivors who sustain cardiac damage might experience long-term effects after their infection has cleared — which suggests that hospitals will need ECG and ultrasound machines to help monitor COVID-19 patients long after the virus has retreated. But right now, that is a battle for tomorrow.