Unlike many newborns, little Shriyan couldn’t spend much time with his mom in the delivery room. Doctors at the Amrita Institute of Medical Sciences in Kerala, India, rushed the critically ill boy to an operating room, where a surgeon was waiting to perform a lifesaving cardiac procedure to correct a rare but fatal heart defect. The doctors taking care of Shriyan didn’t have a crystal ball to know that he needed help. They had something more powerful: prenatal cardiac ultrasound, also known as fetal echocardiography. It allowed them to diagnose the defect while the boy was still in utero — and be ready to act soon after he was born.
Twelve months later, Shriyan is thriving, and Dr. Balu Vaidyanathan, who diagnosed the little boy while he was still in his mom’s belly, has added another success to his growing family of newborns with congenital heart defects who beat the odds. The doctor attributes an important part of that success to prenatal diagnosis, something he’s been evangelizing about for more than a decade. “Ultrasound has tremendous power, especially when you are dealing with an unseen,” he says. “The optimal utilization of this technology is for the benefit of our little babies, so that we can help save precious lives.”
Congenital heart defects occur when the fetal heart doesn’t develop correctly. They are the most common birth defect and a leading cause of infant mortality, especially in developing countries. About 20% of babies born with a heart defect are considered to have “critical” defects, according a 2018 report from India1. They are most likely to die during their first 28 to 30 days, Dr. Balu says. This makes early diagnosis a key to their survival.
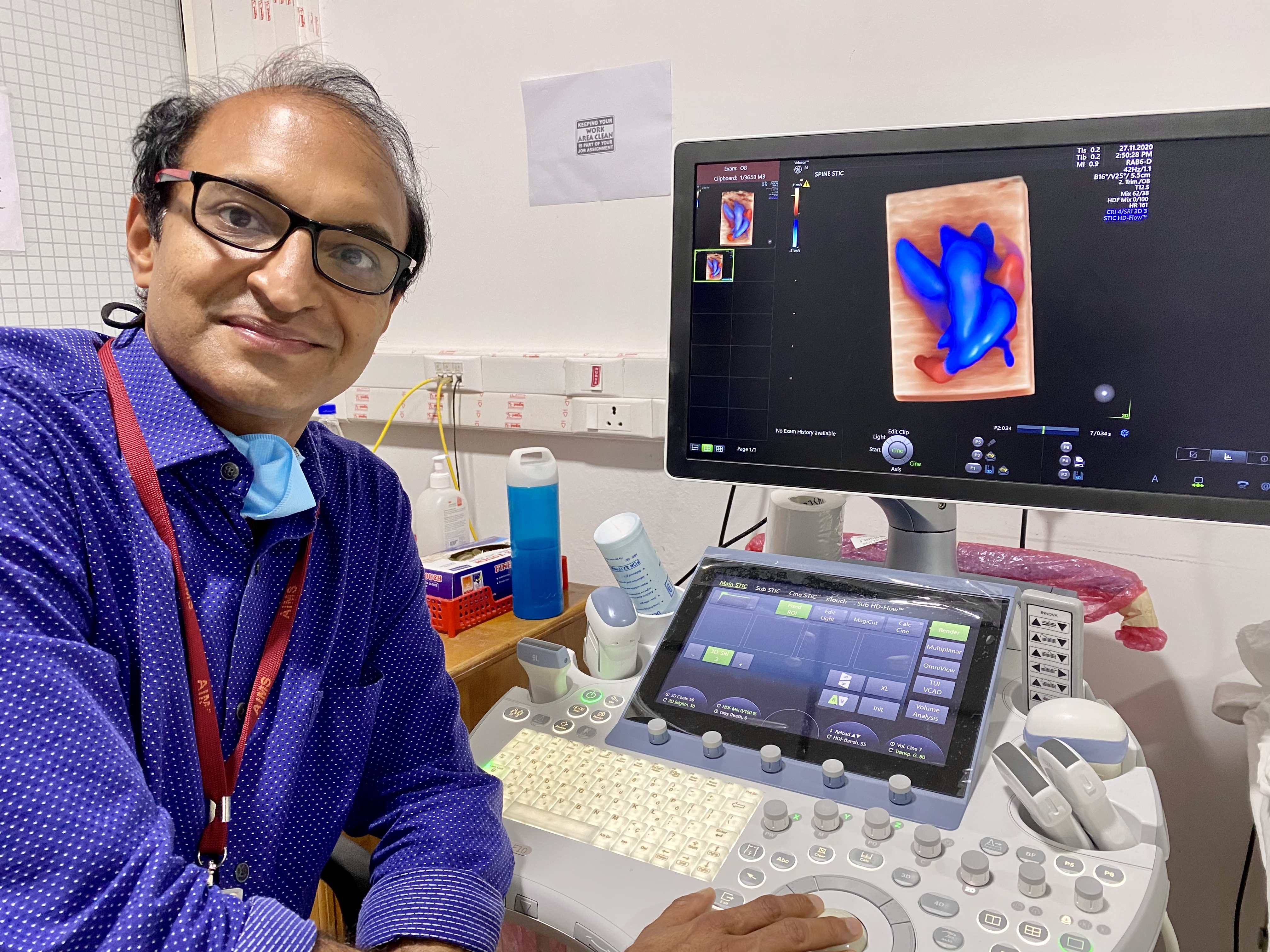
Congenital heart defects are the most common birth defect, particularly in developing nations. Thanks to ultrasound technology, physicians like Dr. Balu Vaidyanathan of Kerala, India, can diagnose these conditions before birth, and be ready to treat their tiny patients promptly after birth. Images credit: GE Healthcare
In countries like India, most heart defects are still diagnosed after birth, using either a clinical exam or a pulse oximeter to measure a newborn’s blood oxygen level. The trouble, Dr. Balu says, is that clinical examinations and oximetry can miss critical defects.
Those are big numbers, considering that India has about 240,000 babies born each year with congenital heart defects1. That means that thousands of babies with deadly heart defects could go undiagnosed until it’s too late.
But early diagnosis can help give newborns like Shriyan a fighting chance. It provides doctors with knowledge about such conditions so they can have a treatment plan ready upon birth.
Shriyan’s mother learned that something could be seriously wrong with her baby’s heart during a routine prenatal exam at 22 weeks. She lived almost nine hours away from Dr. Balu and the pediatric cardiac facility in Kerala where she would eventually give birth. Nevertheless, she traveled to the highly regarded doctor to confirm the diagnosis and develop a treatment plan. That way, Shriyan was born at the right place, the surgeon was ready to operate, and the distance the boy had to move to receive treatment could be measured in meters instead of miles.
Dr. Balu says that, over the past decade, the advent of high-definition ultrasound technology to identify heart defects in utero has been a game changer. In fact, it’s been credited as one of the factors that helped Kerala lower its infant mortality rate from 10 infants per 1,000 as of 2017 to just 7 per 1,000 in the past year2.
The ultrasound machine Dr. Balu uses to examine the tiniest hearts is GE Healthcare’s Voluson E10. It leverages 2D, 3D and color Doppler imaging capabilities to visualize the fetal heart, with the ability to gather more data and use more processing power than previous versions3. (Color Doppler imaging shows the speed and direction of blood flow — blue when the blood flows away from the transducer, red when it flows toward it.) The ultrasound’s software relies on algorithms to improve the quality of images and generate them faster, while also requiring fewer steps for technicians.
The result is clearer images and faster exam times. Doctors can see a fetus’s cardiac structures in high definition, watch them working and assess the level of muscle strain, enabling them to diagnose heart defects during routine second-trimester anatomy scans. Specialists like Dr. Balu can potentially detect anomalies as early as the first trimester of pregnancy using the technology.
Pregnant women then have time to be referred to specialist physicians before the baby is born. A prenatal diagnosis also allows doctors to administer treatments, like stabilizing medications, and plan for surgery immediately after birth.
Early interventions, including use of prenatal ultrasound, help to increase the likelihood of survival — Dr. Balu’s center has a 98% surgical survival rate — and can reduce hospital stays. That, in turn, reduces his patients’ costs by about 25%, the doctor says, which is especially important for lower-income families.
Dr. Balu says that tertiary centers — medical facilities where doctors can perform surgery on a newborn — are also becoming more common, thanks in part to ultrasound’s success, affordability and ease of operation. When he started his practice in pediatric cardiology in the late 1990s, there were four or five tertiary centers in India. Now there are around 30.
[1] Anita Saxena, “Congenital Heart Disease in India: A Status Report,” Indian Pediatrics 55, no 12. (2018):1075–82. PMID: 30745481.
[2] “Our Partners Help to Reduce Infant Deaths in Kerala, India, Children’s HeartLink,” https://childrensheartlink.org/our-partners-help-to-reduce-infant-deaths-in-kerala-india/, accessed January 5, 2021.
[3] GE Healthcare Data on File.