A recent graduate “upcycled” his gown into personal protective equipment for healthcare workers (and inspired others to do the same), researchers found an antibody from a 2003 SARS patient that could be effective against the new coronavirus, and a team of MIT economists crunched the historical numbers and came up with some encouraging results on vaccine development. Read on for more promising news in the fight against COVID-19.
What is it? After attending a virtual ceremony, a newly minted MBA holder from the University of Vermont decided to repurpose his graduation gown into personal protective equipment (PPE) for healthcare workers fighting COVID-19 — and encouraged others to do the same.
Why does it matter? Medics around the world have faced shortages not just of respirator masks but other equipment like hospital gowns. Forming a barrier between clinicians and patients, those items help protect healthcare workers from infection. The Vermont graduate, Nathaniel Moore — who’s also a physician’s assistant at the University of Vermont Medical Center — reasoned that graduation gowns had the right dimensions to be a good substitute. “Graduation gowns are more effective than other PPE alternatives given their length, sleeves, and easy zippered access,” he told CNN.
How does it work? Moore didn’t just donate his own gown; he founded the organization Gowns 4 Good, which encourages other new grads to similarly “upcycle” their garments. In a month, CNN reports, Moore has collected more than 10,000 gowns, and garnered 88,000 requests from front-line workers.
What is it? Researchers have found that an antibody first identified in the blood of a patient who’d recovered from infection with severe acute respiratory syndrome (SARS) in 2003 could be used to treat the current coronavirus.
Why does it matter? Many researchers are studying how coronavirus antibodies could be developed into treatments. A team led by David Veesler of the University of Washington’s School of Medicine and Davide Corti of the Vir Biotechnologies subsidiary Humabs Biomed studied an antibody associated with the 2003 SARS outbreak. Starting with that earlier outbreak allowed them to quickly zero in on an antibody that might have some effectiveness against the current coronavirus, SARS-CoV-2, said Veesler: “This is what allowed us to move so fast compared to other groups.”
How does it work? Veesler et al, who published their findings in Nature, focused on monoclonal antibodies called memory B cells, which form following an infectious illness and “usually remember a pathogen, or one similar to it, that the body has ousted in the past, and launch an antibody defense against reinfection,” according to a University of Washington news release. The antibody that the team identified, called S309, targets the spike protein that enables SARS-CoV-2 to infect human cells, but Veesler warned that there is still work to be done: “We still need to show that this antibody is protective in living systems, which has not yet been done.”

What is it? Though experts have urged patience as scientists race to develop a coronavirus vaccine, a new study from the Massachusetts Institute of Technology illuminates one bright spot: “The probability of success for vaccines is reliably higher than for any other drug development area,” according to economist Andrew Lo, a co-author on the paper, which has been accepted for publication in the Harvard Data Science Review.
Why does it matter? Studying a 20-year span — from 2000 to 2020 — Lo and his co-authors found that “private-sector vaccine-development efforts succeeded in bringing a drug to market 39.6% of the time,” according to MIT, compared to 16.3% of the time for anti-infective therapeutics, including antibiotics. The flip side is that pharmaceutical companies have largely avoided investing in vaccine development, and academic medical centers don’t have the resources to take on that kind of work. “That’s worrisome, because we know for a fact that these diseases are real threats, and yet there’s been relatively little attention paid to them,” Lo said.
How does it work? “The reason we wrote this paper is to bring more awareness to this situation. Now that we’ve experienced the deadly consequences of a pandemic, the hope is that governments around the world — and it really has to be governments — will pay more attention,” Lo said. “As the saying goes, ‘crisis is a terrible thing to waste,’ so we need to take advantage of this opportunity to come up with a more enduring solution, not just for this pandemic, but for all future pandemics.”
What is it? The way the immune system responds to infection with SARS-CoV-2 is “diverse and unpredictable,” writes Tufts University professor Alexander Poltorak in The Conversation, which makes the disease challenging to treat — particularly when the immune system overreacts. Poltorak, who studies innate immune responses, is searching for ways to prevent that.
Why does it matter? Poltorak is focusing particularly on cytokine storms, which result when white blood cells produce proteins called cytokines to fight infection. The cytokines induce a number of responses that the immune system uses to fight infection— like elevated heartbeat and body temperature — but they can grow out of control. A “storm,” writes Poltorak, is when “a flood of white blood cells ... enter the lungs, which in turn summon more immune cells that target and kill virus-infected cells. The result of this battle is a stew of fluid and dead cells, and subsequent organ failure.”
How does it work? How, then, to forestall a cytokine storm? That’s what Poltorak and his colleagues are studying, including antibodies that might be effective in “breaking the vicious cycle” of the storms. Some cytokine-blocking drugs are now in clinical trials to test their effectiveness against COVID-19; learn more here.
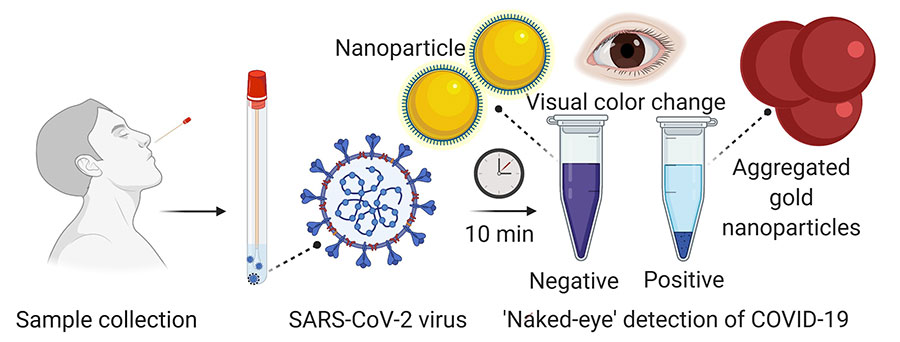
What is it? Scientists at the University of Maryland School of Medicine (UMSOM) developed a diagnostic test for COVID-19 that returns results in 10 minutes and doesn’t require the use of any special lab equipment.
Why does it matter? Public health officials say that testing and tracing will be a crucial means of controlling the spread of the new coronavirus until a vaccine can be developed and distributed, but such tests in the U.S. have been dogged with concerns over accuracy. Dipanjan Pan, leader of the UMSOM study, said, “The accuracy of any COVID-19 test is based on being able to reliably detect any virus. This means it does not give a false negative result if the virus actually is present, nor a false positive result if the virus is not present. Many of the diagnostic tests currently on the market cannot detect the virus until several days after infection. For this reason, they have a significant rate of false negative results.”
How does it work? Describing their work in the journal ACS Nano, Pan and colleagues devised an RNA-based test that uses plasmonic gold nanoparticles to detect the presence of the virus in a nasal or saliva swab; when a molecule attached to the gold nanoparticles detects a particular protein associated with the coronavirus in a liquid reagent, the nanoparticles change the color of the liquid. Pan said that the preliminary results suggest the test can detect the presence of viral RNA material as early as the first day of infection, but further study is needed for confirmation.





