Decoding Cancer In Seconds
[embed width="600"]https://www.youtube.com/watch?v=DNfG0dgFQ0Q[/embed]
What is it? Researchers at the University of Austin in Texas have developed a small, disposable, pen-like device that can identify cancer during surgery “in about 10 seconds.” That’s “more than 150 times as fast as existing technology,” according to UT News. The team reported that the device was 96 percent accurate in tests.
Why does it matter? The tool gives surgeons “precise diagnostic information about what tissue to cut or preserve, helping improve treatment and reduce the chances of cancer recurrence,” UT News wrote. The technology “could vastly improve the odds that surgeons really do remove every last trace of cancer during surgery,” says Livia Schiavinato Eberlin, an assistant professor of chemistry at UT Austin who designed the study and led the team.
How does it work? The pen uses mass spectrometry to analyze metabolites, small molecules produced by cells. “Cancer cells have dysregulated metabolism as they’re growing out of control,” Eberlin said. “Because the metabolites in cancer and normal cells are so different, we extract and analyze them with the MasSpec Pen to obtain a molecular fingerprint of the tissue.”
Top image: The MasSpec Pen rapidly and accurately detects cancer in humans during surgery, helping improve treatment and reduce the chances of cancer recurrence. Image and caption credit: University of Texas at Austin.
About Face
 "We set out to do this study to prove that your genome codes for everything that makes you, you,” said HLI's J. Craig Venter. Image credit: Getty Images.
"We set out to do this study to prove that your genome codes for everything that makes you, you,” said HLI's J. Craig Venter. Image credit: Getty Images.What is it? J. Craig Venter and a team of researchers from Human Longevity, Inc. (HLI) used DNA data from more than 1,000 people and machine learning to generate individual faces and physical features like eye, skin color and face shape. "We set out to do this study to prove that your genome codes for everything that makes you, you,” Venter said. “This is clearly a proof of concept with a limited cohort but we believe that as we increase the numbers of people in this study and in the HLI database to hundreds of thousands we will be able to accurately predict all that can be predicted from individuals' genomes.
Why does it matter? The study “offers novel approaches for forensics,” but the authors believe “the work has serious implications for data privacy, de-identification and adequately informed consent,” according to PhysOrg. “The team concludes that much more public deliberation is needed as more and more genomes are generated and placed in public databases.”
How does it work? The team sequenced the genomes of “1,061 ethnically diverse people ranging in age from 18 to 82.” It also collected “phenotype data in the form of 3-D facial images, voice samples, eye and skin color, age, height, and weight.” The team fed the information to a machine-learning algorithm to find “an optimal combination of all predictive models to match whole-genome sequencing data with phenotypic and demographic data.”
Methuselah Fruit Flies
 UCLA scientists slowed down aging in fruit flies and extended their lifespan by as much as 20 percent. Image credit: Getty Images.
UCLA scientists slowed down aging in fruit flies and extended their lifespan by as much as 20 percent. Image credit: Getty Images.What is it? UCLA scientists slowed down aging in fruit flies and extended their lifespan by as much as 20 percent by removing damaged mitochondria, the miniscule generators that supply cells with energy.
Why does it matter? UCLA reported the technique “could eventually lead to a way to delay the onset of Parkinson’s disease, Alzheimer’s disease, cancer, stroke, cardiovascular disease and other age-related diseases in humans.”
How does it work? The team observed that when fruit flies get a month old and reach middle age, their mitochondria “become larger and elongated,” hindering the cell’s ability to get rid of them. The damaged mitochondria can become toxic and lead to age-related diseases. The team found a way to break them up to get rid of them. UCLA reported that when they did, “the flies became more active and more energetic and had more endurance. Following the treatment, female flies lived 20 percent longer than their typical lifespan, while males lived 12 percent longer, on average.”
Team Kills Brain Cancer With Zika
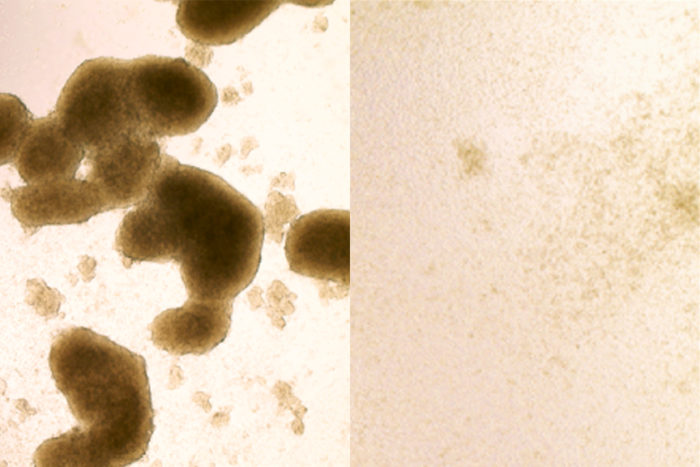 Brain cancer stem cells (left) are killed by Zika virus infection (image at right shows cells after Zika treatment). A new study shows that the virus, known for killing cells in the brains of developing fetuses, could be redirected to destroy the kind of brain cancer cells that are most likely to be resistant to treatment. Image and caption credit: Zhe Zhu/Washington University School on Medicine in St. Louis.
Brain cancer stem cells (left) are killed by Zika virus infection (image at right shows cells after Zika treatment). A new study shows that the virus, known for killing cells in the brains of developing fetuses, could be redirected to destroy the kind of brain cancer cells that are most likely to be resistant to treatment. Image and caption credit: Zhe Zhu/Washington University School on Medicine in St. Louis.What is it? Zika virus can kill cells in the brains of developing fetuses. But it also can destroy brain cancer resistant to treatment, according to new research carried out at Washington University and the University of California San Diego.
Why does it matter? Washington University reported that turning “the lethal power of the virus” against glioblastoma, a kind of brain cancer, could potentially “improve people’s chances” against the disease. “We showed that Zika virus can kill the kind of glioblastoma cells that tend to be resistant to current treatments and lead to death,” said Michael Diamond, a professor at Washington University School of Medicine and the study’s co-senior author.
How does it work? The team said that a small population of cancer cells often survive the standard treatment — a combination of surgery, radiation and chemotherapy treatment — and keep dividing. “The standard treatment kills the bulk of the tumor cells but often leaves the stem cells intact to regenerate the tumor,” the university reported. “Zika virus attacks the stem cells but bypasses the greater part of the tumor.” Senior co-author Milan Chheda said that the team saw “Zika one day being used in combination with current therapies to eradicate the whole tumor.”
There’s An App For Concussions
[embed width="600"]https://www.youtube.com/watch?v=sZwgpz4s8Jw[/embed]
What is it? Researchers at the University of Washington are building PupilScreen, “the first smartphone app that is capable of objectively detecting concussion and other traumatic brain injuries.”
Why does it matter? The app “aims to generate objective and clinically relevant data that anyone on the sidelines could use to determine whether a player should be further assessed for concussion or other brain injury,” according to the university. “Right now, the best screening protocols we have are still subjective, and a player who really wants to get back on the field can find ways to game the system,” said Shwetak Patel, an engineering and computer science professor at the University of Washington.
How does it work? The app uses a form of AI to detect changes captured by the camera in the pupil’s response to light and “quantify changes imperceptible to the human eye.” The team envisions a smartphone camera interface that enables a user to “simply hold the phone up and use the flash,” said lead author Alex Mariakakis, a doctoral student in the university’s Paul G. Allen School of Computer Science and Engineering. “We want every parent, coach, caregiver or EMT who is concerned about a brain injury to be able to use it on the spot without needing extra hardware.”