A Zombie Pox Virus
 Top: Scientists in Canada have created a man-made replica of the extinct horsepox virus. Above: The research raised alarm that someone might be able to synthesize the virus’ lethal cousin, smallpox (above), which the World Health Organization declared eradicated in 1980. Images credit: Getty Images.
Top: Scientists in Canada have created a man-made replica of the extinct horsepox virus. Above: The research raised alarm that someone might be able to synthesize the virus’ lethal cousin, smallpox (above), which the World Health Organization declared eradicated in 1980. Images credit: Getty Images.What is it? A team of scientists led by David Evans, a virologist from the University of Alberta, have created a man-made replica of the extinct horsepox virus. The research raised alarm that someone might be able to synthesize the virus’ lethal cousin, smallpox, which the World Health Organization declared eradicated in 1980. The results were reported in the journal Science.
Why does it matter? Science wrote that Evans hoped the research would “help unravel the origins of a centuries-old smallpox vaccine and lead to new, better vaccines or even cancer therapeutics.” Tom Inglesby, director of the Center for Health Security at Johns Hopkins University’s Bloomberg School of Public Health, called in a blog post for international guidelines to direct such research. “We need agreed-upon norms that will help guide countries and their scientists regarding work that falls into this category, and high-level dialogue regarding the necessary role of scientific review, guidance, regulation for work that falls into special categories of highest concern.”
How did they do it? The work hasn’t been published, but Science reported that the team mail-ordered “DNA fragments, each about 30,000 base pairs in length, from a company that synthesizes DNA commercially and then “stitch[ed] together the 212,000-base-pair horsepox virus genome.” The project reportedly cost $100,000.
Horsing Around With CRISPR
 Wired called the project “an interesting—if slightly gimmicky—way to show off CRISPR's power to turn living cells into digital data warehouses.” Image credit: Getty Images.
Wired called the project “an interesting—if slightly gimmicky—way to show off CRISPR's power to turn living cells into digital data warehouses.” Image credit: Getty Images.What is it? A group of Harvard researchers used the CRISPR-Cas9 gene-editing tool to encode a pixelated GIF of a jockey riding a galloping horse into a living E. coli bacteria.
Why does it matter? The team wrote in the journal Nature that encoding “a short movie” in the bacteria demonstrated “that that this system can capture and stably store practical amounts of real data within the genomes of populations of living cells.” Harvard geneticist and co-author of the paper Jeff Nivala told Wired that the teams “real goal [was] to enable cells to gather information about themselves and to store it in their genome for us to look at later.” He believes the technology could be used to record chatter between brain cells.
How does it work? The team wrote that CRISPR-Cas9 had “the potential to write arbitrary information into the genome.” Wired called the project “an interesting—if slightly gimmicky—way to show off CRISPR's power to turn living cells into digital data warehouses.”
A Helping Hand
[embed width="800"]https://www.youtube.com/watch?v=ZJJnrybwcqo[/embed]
What is it? Engineers at the University of California, San Diego have built “a smart glove that wirelessly translates the American Sign Language alphabet into text and controls a virtual hand to mimic sign language gestures.” Future applications of the technology could include “virtual and augmented reality to tele-surgery, technical training and defense.”
Why does it matter? “Our ultimate goal is to make this a smart glove that in the future will allow people to use their hands in virtual reality, which is much more intuitive than using a joystick and other existing controllers,” the team said in a press release. “This could be better for games and entertainment, but more importantly for virtual training procedures in medicine, for example, where it would be advantageous to actually simulate the use of one’s hands.”
How does it work? The engineers said they spent less than $100 to build the glove from stretch materials, printable electronics and a leather athletic glove. “The sensors change their electrical resistance when stretched or bent,” the team said. “This allows them to code for different letters of the American Sign Language alphabet based on the positions of all nine knuckles. A straight or relaxed knuckle is encoded as ‘0’ and a bent knuckle is encoded as ‘1.’ ”
This AI Can Spot Concussions Years After Injury
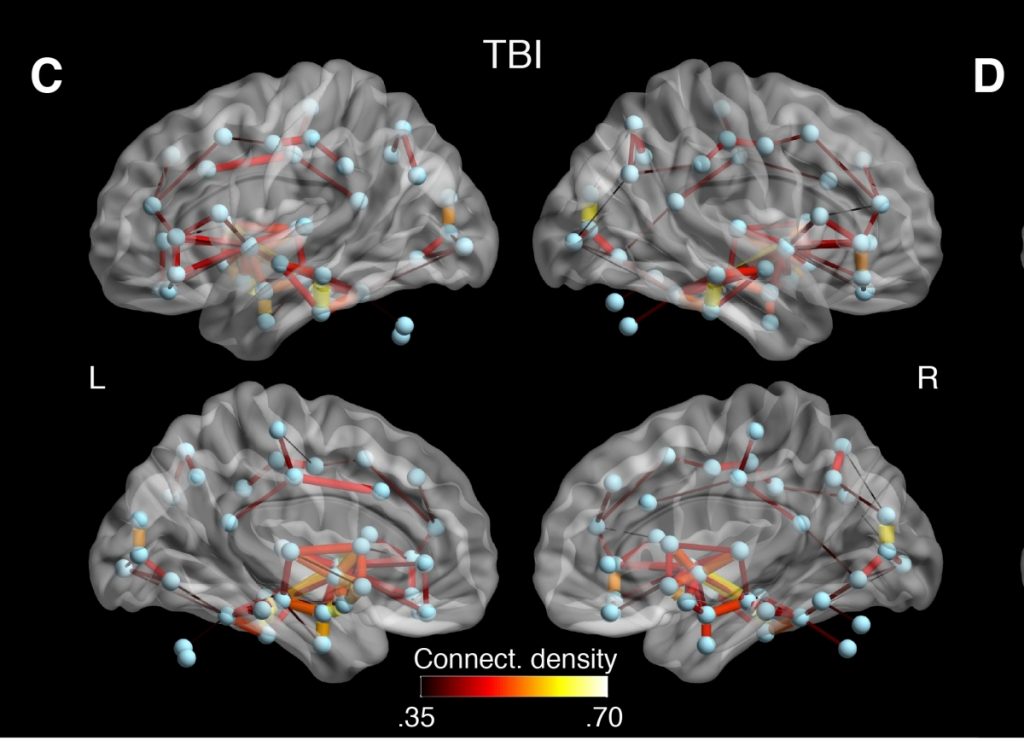 The AI, which “learned” to spot “differences between the brain of a healthy athlete versus the brain of a previously concussed athlete” with 90 percent accuracy. Image credit: McGill University.
The AI, which “learned” to spot “differences between the brain of a healthy athlete versus the brain of a previously concussed athlete” with 90 percent accuracy. Image credit: McGill University.What is it? Canadian researchers working in Montreal have developed an AI that can spot symptoms of a concussion in athletes “years after it occurred.”
Why does it matter? The team wrote that concussion symptoms “may linger for years” and that these “long-term effects can be equally hard for patients” as problems experienced immediately after the head injury happened. “It is unacceptable that no objective tools or techniques yet exist to diagnose them, not to mention the sheer lack of scientifically valid treatment options,” said Sebastien Tremblay, the first author of the paper, which was published in the European Journal of Neuroscience. “With our work, we hope to provide help to the vast population of former athletes who experience neurological issues after retiring from contact sport.”
How does it work? The team first picked 15 “former university athletes between the ages of 51 and 75 who played contact sports such as ice hockey and American football” and had suffered a concussion. They also selected a control group of the same size. They ran numerous tests on the groups, including MRIs, and fed the data to the AI, which “learned” to spot “differences between the brain of a healthy athlete versus the brain of a previously concussed athlete” with 90 percent accuracy.
Brain Power
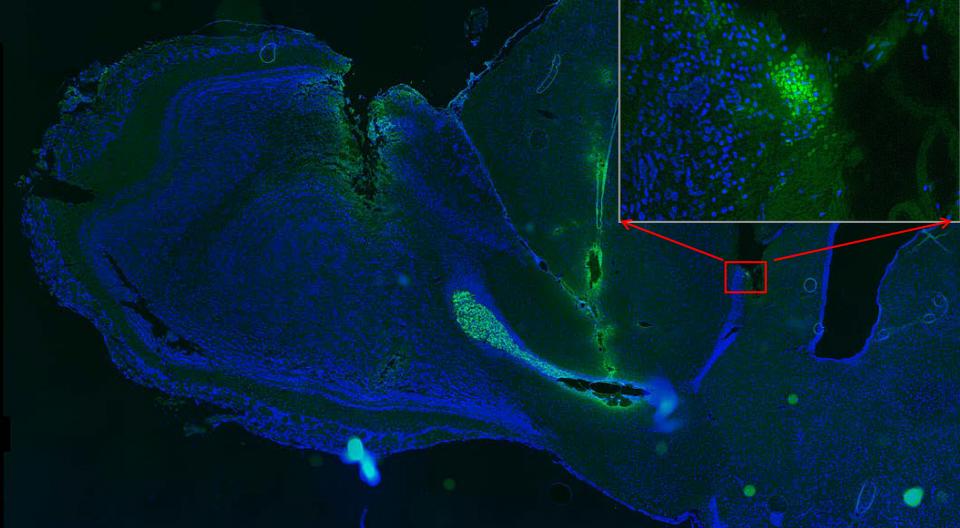 Transplants of neural stem cells might be used to treat brain injuries, but how to get them to the right location? UC Davis researcher Min Zhao and Junfeng Feng, a neurosurgeon at Ren Ji Hospital, Shanghai, showed that they can steer transplanted stem cells (green, in inset on right) to one part of a rat’s brain using electrical fields. caption crediImage credit: Junfeng Feng.
Transplants of neural stem cells might be used to treat brain injuries, but how to get them to the right location? UC Davis researcher Min Zhao and Junfeng Feng, a neurosurgeon at Ren Ji Hospital, Shanghai, showed that they can steer transplanted stem cells (green, in inset on right) to one part of a rat’s brain using electrical fields. caption crediImage credit: Junfeng Feng.What is it? A team led by a researcher at the University of California, Davis found a way to use electric fields to “guide neural stem cells transplanted into the brain toward a specific location.” The research “opens possibilities for effectively guiding stem cells to repair brain damage.”
Why does it matter? “One unmet need in regenerative medicine is how to effectively and safely mobilize and guide stem cells to migrate to lesion sites for repair,” said Min Zhao, a professor at the UC Davis medical school’s Institute for Regenerative Cures. “Inefficient migration of those cells to lesions is a significant roadblock to developing effective clinical applications.” Zhao said that “electrical mobilization and guidance of stem cells in the brain therefore provides a potential approach to facilitate stem cell therapies for brain diseases, stroke and injuries.”
How does it work? Zhao and his research partner Junfeng Feng found a way to guide transplanted stem cells inside a rat’s brain and make them “swim ‘upstream’ against the fluid flow and natural cues and head for other locations within the brain.” They reported that the “cells were still in their new locations weeks or months after treatment.”





