GE Healthcare's AIR Recon DL software separates signal from noise without compromising diagnostic quality or increasing scan time.
Taking the perfect selfie is an exercise of trial and error. We snap, study and delete, until we finally capture ourselves in our best light. Now imagine the difficulty of obtaining a high-quality image in a nonconventional medium: The inside of the body.
That is the perennial challenge for radiologists who use magnetic resonance (MR) scanners to see deep inside the internal structures of the human body and make diagnoses. But it is not poor light that can mar their picture, just a bad signal. To tackle this troublesome issue, GE Healthcare is building artificial intelligence (AI) software designed to cut through the noise to deliver razor-sharp anatomical imaging. This meaningful quality boost can enable faster, more accurate patient diagnoses and, in turn, better outcomes.
First, a quick primer on modern MR technology. MR scanners are giant, tube-shaped machines used by radiologists to image organs, muscle and other soft tissues, as well as brain activity. Unlike computed tomography (CT) and X-ray machines, MR scanners do not use ionizing radiation to do their job. They instead produce strong magnetic fields that jiggle hydrogen atoms in the body’s water and fat. Those atoms then emit radio signals which are detected by the scanner and transformed into a digital image. Radiologists can read these images to scrutinize the body’s soft tissue and organs, helping to diagnose diseases or injuries.
But those valuable signals compete for image space with a constant racket of background thermal and electrical noise. That is because the human body and the apparatus of the MR scanner are also broadcasting tiny radio waves. These miniature broadcasts of noisy signals can conceal problems in the MR images and deceive the trained eye. “Noise obscures anatomy and pathology, making reads slow and uncertain,” said Dr. Marc Lebel, scientist at GE Healthcare.
Sharp transitions in signals are also a bugaboo for radiologists. These transitions can cause a phenomenon called “Gibbs ringing,” which appears as faint lines on MR images. Lebel said Gibbs ringing raises a red flag that something is missing: “It is always evidence that you have not captured all the detail in an image. Instead of sharp edges where you should have detail,” he said, “you get ringing around the edges.”
Such flaws are a real problem for clinicians. Dr. Javier Villanueva-Meyer, an assistant professor of clinical radiology at the University of California, San Francisco, said image quality is crucial to radiologists because MR imaging is often “the gold standard” for diagnosis in branches of medicine such as neuroimaging, where doctors image the brain and nervous system. “Sampling tissue for diagnosis and treatment monitoring is a costly, invasive alternative with the potential for significant morbidity.”
Radiologists have some tricks to reduce noise, purge artifacts and exorcise their Gibbs ringing. They can perform longer-duration scans to boost the signal-to-noise ratio (SNR) or resolution in an MR image. But prolonging an MR scan can be taxing for patients prone to feeling anxious in confined spaces. Longer scans also eat into a clinician’s demanding schedule and a hospital’s revenue. On the flip side, shorter scans typically deliver lower SNRs, eroding diagnostic confidence. Villanueva-Meyer said there is a risk of clinically significant results being “underestimated or undiagnosed” with “fast MR” scans.
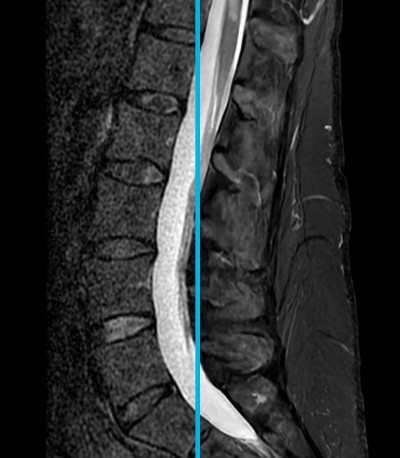
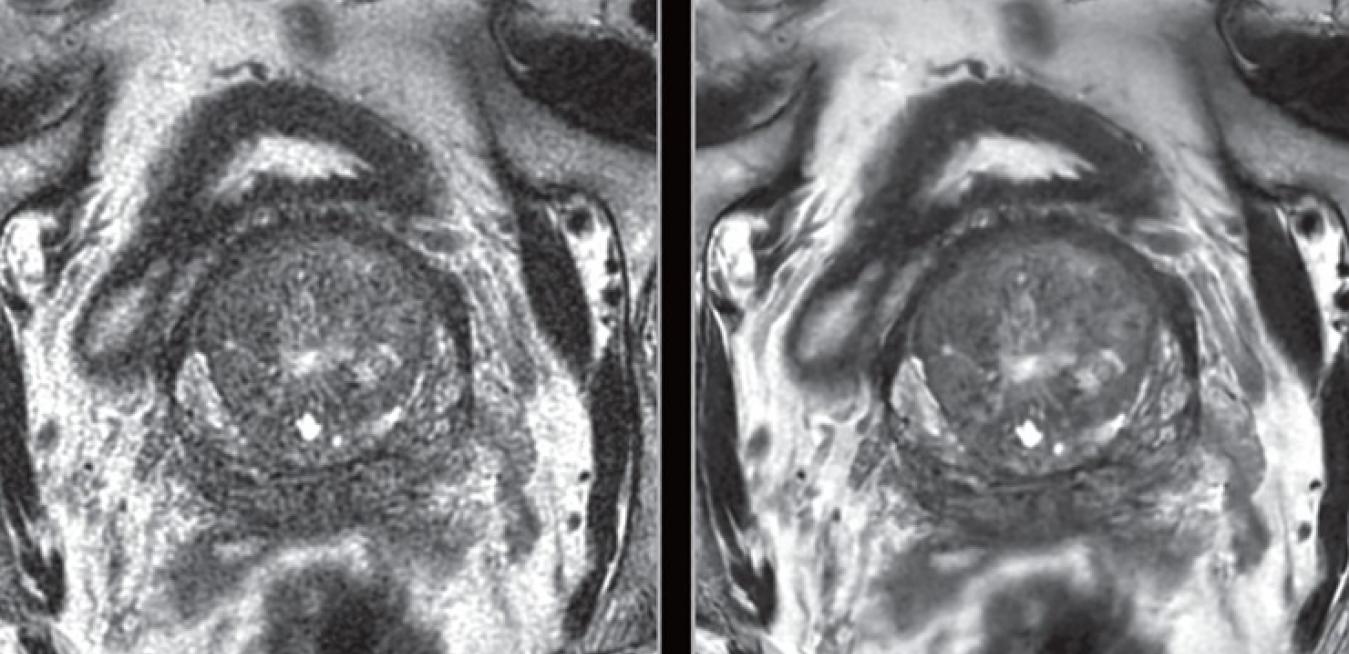
Radiologists can also filter out noise and Gibbs ringing with a smoothing technique that combines neighboring signals. But this, too, is no panacea for the problem: While they successfully reduce noise and ringing, they also sacrifice some signal, which Lebel said “blurs out the detail.”
Now artificial intelligence can help answer the call of both radiologist and patient. AIR Recon DL is a software built by GE Healthcare that is currently 510(k) pending with the U.S. Food and Drug Administration. It is designed to separate signal from noise without compromising diagnostic quality or increasing scan time, according to Lebel. GE built the AI by using its Edison AI platform to feed the computer algorithms with tens of thousands of images. The software uses an array of some 100,000 image filters that analyze clinical images to identify likely patterns of noise and Gibbs ringing.
But there’s more. Besides just purging the images of noisy patches, the software’s neural network is designed to fill blank spots with plausible anatomical detail. Lebel likens it to a tiny master artist inside the human body, painting a detailed impression wherever they see a gap. Unlike many forms of healthcare AI applied as post-processing techniques, AIR Recon DL has the potential to polish up images in real time. “We’ve plugged the AI straight into our image reconstruction pipeline, so it’s right there instantly making images,” Lebel said.
The software was unveiled in early December at the Radiological Society of North America’s (RSNA) annual meeting, the world’s largest gathering of radiologists, in Chicago. But this AI is already delivering tangible results with multiple users who have a research prototype version.
“The major benefits [observed using the prototype version] included ease of implementation into current workflow, minor protocol modifications for the technologist, and the potential for faster scans,” said Villanueva-Meyer. He said the potential for faster scans can help deliver a better patient experience and, of course, allow a doctor to see more patients.
Dr. Pascal Roux, a radiologist at Centre Cardiologique du Nord (CCN) in Paris, said the software’s shorter acquisition time—the time it takes the machine to produce an image—will allow him to add up to six more patients in a 12-hour day. And that progress certainly warrants making some noise.