With an aging population this global disease burden is only set to rise, and against a backdrop of widespread austerity where health systems everywhere are being called upon to achieve more for less. There has never been greater pressure to justify value for money in healthcare.
Defining ‘Value for Money’
Assessing value for money in any sphere need not be a subjective exercise. While the definition of value will vary according to regions, populations, health needs, and available resources, clinically and economically relevant innovation can be the stable factor.
As Victor Fuchs says in a 2010 NEJM editorial How to Think about Future Health Care Spending:“[I]t is fiscally irresponsible to continue to accept innovations regardless of cost, even if they pass tests of safety and efficacy—and it is particularly irresponsible when the interventions are provided at public expense.”
Health technology assessment agencies undertake specific and robust evaluations to determine value for money based on returns to society. In light of this, the value of informed Health Technology Assessments such as those performed by UK’s National Institute for Clinical Excellence [NICE] cannot be underestimated. NICE is a leading example and others exist, both formally and informally, around the world. They consider not only costs but also the broader issue of affordability.
Affordability accounts for full costs including acquisition, implementation, operation, and maintenance within a regional context. To make affordable interventions, it is necessary to fully understand the health priorities of the region in addition to available infrastructure and appropriate resourcing.
An assessment of value for money must take into consideration what the investment is designed to achieve. Further, new medical technology must be considered in conjunction with health care worker and training needs, especially in developing markets.
Ultimately, healthcare professionals around the world rely on medical devices to provide effective preventive, diagnostic, therapeutic, and rehabilitative services. There is mounting evidence that investing in medical devices reduces healthcare expenditure over the long term and contributes towards better patient outcomes.
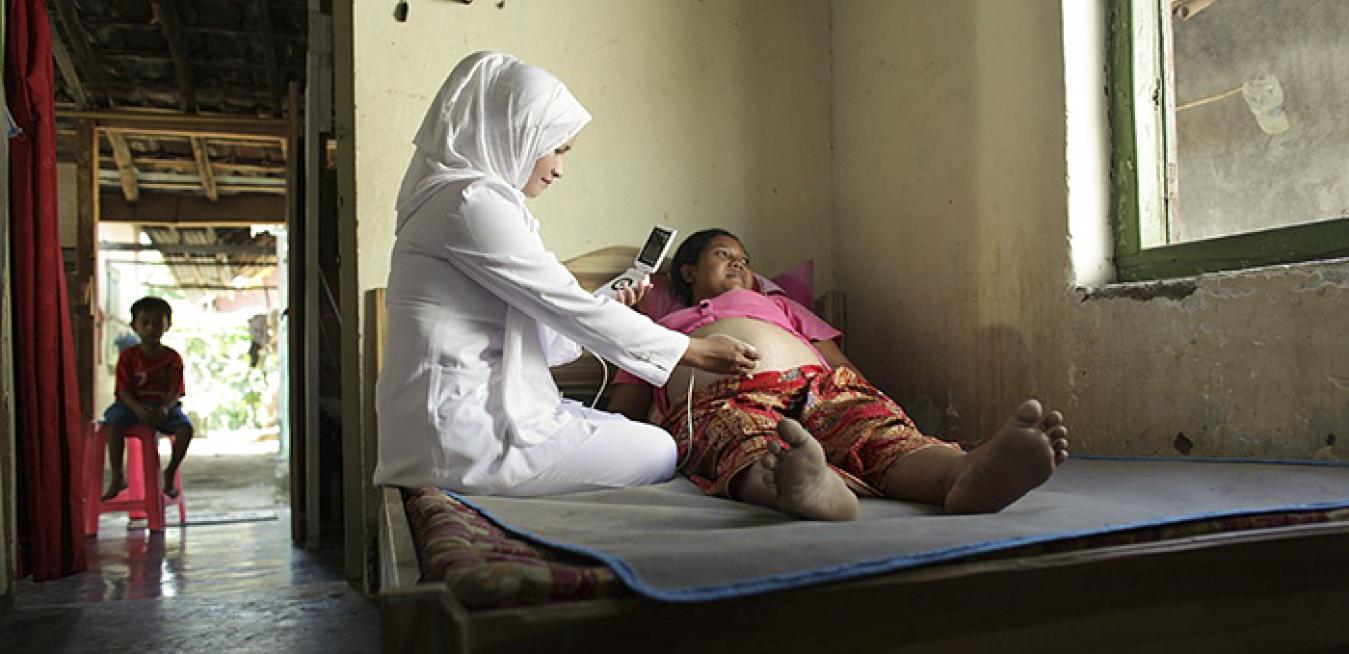
Doctor uses GE’s Vscan, a pocket-sized ultrasound device, to check on rural patient. The device is used worldwide in developing and developed countries.
There is also growing evidence of the value of early diagnosis—detecting and treating disease earlier when it may be more responsive to treatment and corollary conditions can be reduced or avoided. The social and economic impact of early diagnosis delivers value to patients, health systems and governments. With the right technology available, officials can deliver salient clinical and economic returns, ensuring true value to populations and regions around the world.
Investing in the Right Technology
Population health needs and the resources available to meet them can be understood at one of the most elemental levels of definition, income available. Regions with lower income per capita are faced with challenges including not only of infectious disease and maternal and infant mortality but also issues of aging populations and non-communicable diseases (NCDs). These areas require the highest quality technology available but must address available infrastructure and workforce resources. New technologies must be tailored not only to population health needs but also to the environmental context in which the technologies will be placed.
GE’s focus on reverse innovation means products can be designed to meet the needs of developing markets while also being of value for developed countries. A particular challenge for developing countries is providing healthcare in rural areas with little access to electricity and qualified healthcare workers. GE’s Vscan helps address these challenges.
Originally developed for low resource settings, Vscan is a compact portable visualization tool with ultrasound technology that provides a non-invasive look inside the body for immediate visual validation of what a clinician can feel or hear. The additional information helps optimize the course of treatment for a patient and reduces the time required for diagnosis. The device is small, lightweight and solar-charged to provide a full day’s worth of patient exams in a remote rural setting.
At only a fraction of the cost of a high-end unit, the Vscan is being used in by paraprofessionals in Indonesia, Tanzania, Ghana, and Bangladesh, attracting more mothers to the formal health system and increasing antenatal attendance and institutional delivery. Meanwhile, in developed countries, the portability and clear images produced by these devices are helping to change the way heart patients are tested in hospital and in outpatient clinics. Soon every GP clinic could feature one.
GE is also developing technologies specifically geared to newborn needs in low-resource settings. The Lullaby Warmer is another example of reverse innovation at work. The device, which is 70 percent cheaper than traditional models and includes pictorial directions understood in any language, has been successful in rural areas of India as well as in developed countries. ,The Lullaby LED Phototherapy, which treats neo-natal jaundice, was initially designed for the Indian market by GE’s R&D Center in Bangalore to withstand power outages, voltage fluctuations, high levels of dust and pollution, and intensive equipment use common in that region. Now that device is used worldwide in developing and developed countries alike.
A number of these technologies are now on the WHO Compendium of Innovative Health Technologies list, which is part of an initiative to promote the development and adoption of relevant technologies.
Technology Investment in Developed Countries
Altogether, NCDs caused 36 million deaths in 2008, accounting for more than three out of five deaths worldwide and contributing toward half of global disability. As NCDs such as coronary heart disease and stroke have emerged “relatively unnoticed” in the developing world, it would be fair to assert these diseases pose great risks to health, economy and society globally.
Investing in technologies in more developed areas remains imperative. For example, many nations are searching for effective and cost-efficient ways to diagnose, treat and manage an increase in the incidence of cardiovascular disease, or CVD, a problem with a disproportional impact on low-and-moderate-income nations. For cost-constrained healthcare systems, one question to be asked is this: Can technologically advanced diagnostics serve as an accurate gatekeeper to more expensive and invasive procedures such as those used in evaluating coronary artery disease (CAD)?
A number of large, multicenter trials, systematic reviews and economic studies have already addressed this question. For evaluating low-risk patients with chest pain, coronary CT angiography is proving itself to be a desirable and cost-efficientfirst-line test for CAD.
An Investment, Not Only a Cost
The economic implications of NCDs are staggering. It is estimated that 50 percent of NCD-related deaths are during “productive years,” representing a significant cost to both governments and the commercial sector. The theory underpinning this argument is that healthier individuals produce more output per hour worked leading to increased labor productivity. A Harvard study has shown that a one-year improvement in a population’s life expectancy contributes towards an increase of output by 4 percent. On the flip side, productivity losses associated with disability, unplanned absences and increased accidents account for as much as 400% more than the cost of treatment.
New technology is going to play an ever increasing role in our ability to solve the healthcare challenges of our age. It is essential that health systems and governments around the globe recognise the total value that technological investment can bring to save lives and increase efficiency, as well as secure wider economic prosperity.
Healthcare is an investment, not just a cost. By investing in technology infrastructure, a country will have not only a healthier workforce but also a healthier economy.
Central to this proposition is the adoption of the right technologies and training solutions to meet the needs of individual countries and healthcare settings, a partnership approach among governments, academia and industry, and a legislative climate that encourages the development and adoption of appropriate innovations.
Karim Karti is vice president and chief marketing officer at GE Healthcare. A version of this article first appeared in Global Health Diplomacy magazine.
Spending Money, Saving Lives was originally published on Ideas Lab