Desperate to find a treatment, her parents enrolled her in an experimental trial at The Children’s Hospital of Philadelphia (CHOP) in early 2012. CHOP’s doctors drew her blood and collected some of Emily’s T lymphocytes — white blood cells that form the backbone of the human immune system. The team then reprogrammed the cells by altering their DNA so they would recognize and kill Emily’s cancer. Doctors injected them back into Emily’s bloodstream, where the cells multiplied and wiped out the disease.
Emily has remained cancer-free since. She’s become the poster child for a new type of personalized medicine called cellular immunotherapy, a type of regenerative medicine that seeks to fix faulty cells and tissues by reengineering their DNA and restoring their normal function. “We are on the cusp of a revolution in medicine,” says Phil Vanek, general manager for cell therapy technologies at GE Healthcare. “These are living drugs. The reprogrammed cell itself becomes the treatment that gets reintroduced to the patient. Ordinary drugs wear off after we take them, but regenerative medicine can have a durable effect. It can restore a function that was lost or, someday, give our cells one they never had.”
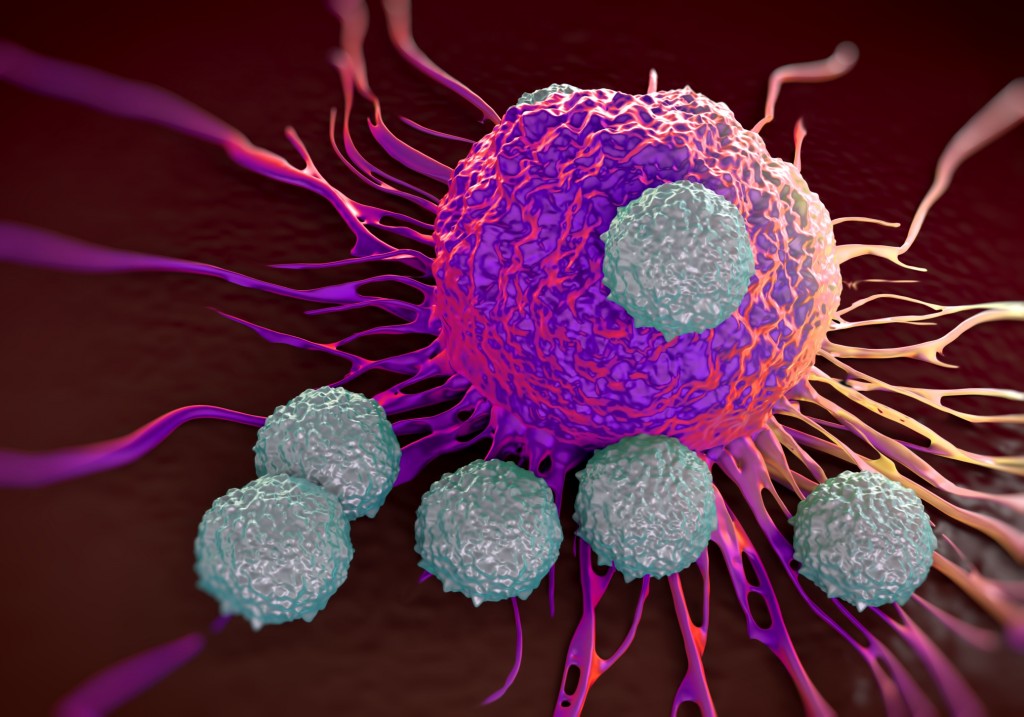 Top image: Canadian Prime Minister Justin Trudeau (leaning) during a tour of CCRM's labs on Wednesday. CCRM President and CEO Michael May is standing on the right. Image credit: GE Reports Above: T-cells attacking a cancer cell. Image credit: Getty Images
Top image: Canadian Prime Minister Justin Trudeau (leaning) during a tour of CCRM's labs on Wednesday. CCRM President and CEO Michael May is standing on the right. Image credit: GE Reports Above: T-cells attacking a cancer cell. Image credit: Getty ImagesGE helped design the bioreactor CHOP doctors used to grow Emily’s cancer-trained T cells and has a number of products and services used in cell therapy manufacturing today. However, the company doesn’t want to innovate in a vacuum. Vanek believes the more collaboration he and his team can encourage in the industry, the faster these therapies get to the market. That’s why GE and the Canadian government will each invest CA$20 million in a new cell therapy research and process development hub in Toronto led by Canada’s Centre for Commercialization of Regenerative Medicine (CCRM). Canadian Prime Minister Justin Trudeau announced the news this week.
The new center will bring together researchers, universities, drug manufacturers and technology companies like GE to speed up the development and production of cell therapies and make them available to patients more quickly. “Cell therapy has the potential to cure everything from cancer to diabetes,” Vanek says. “But we need to make it affordable and scalable. In this era of increasing scrutiny of medical costs and reimbursement, we have to help our customers achieve a reasonable cost of goods.”
![GE's W25 _Xuri_Cell_Expansion_System[1]](https://www.ge.com/news/sites/default/files/Reports/uploads/2016/01/13120914/GEs-W25-_Xuri_Cell_Expansion_System1-1024x828.jpg) GE's Xuri cell expansion system used for growing cells. Image credit: GE Healthcare Life Sciences
GE's Xuri cell expansion system used for growing cells. Image credit: GE Healthcare Life Sciences Today the city boasts a rich research and bioengineering ecosystem. Since CCRM opened in 2011, the not-for-profit has brought together 50 partners, including academic teams, pharmaceutical and technology companies, investors and regulators. The new center will be located inside Toronto’s 1-million-square-foot MaRS Discovery District, sharing the space with Facebook, Johnson & Johnson’s JLabs, Autodesk and venture investors. The main University of Toronto campus, a cluster of hospitals and the Ontario legislative assembly are right next door. “We need to integrate existing technology to break through manufacturing bottlenecks and make cell therapy affordable and available,” says CCRM President and CEO Michael May. “This rich environment will help us validate new clinical technologies and turn them into lucrative products.”
 The new center will be located inside Toronto’s 1-million-square-foot MaRS Discovery District. Image credit: GE Reports
The new center will be located inside Toronto’s 1-million-square-foot MaRS Discovery District. Image credit: GE ReportsGE, one of CCRM’s founding partners, will play an anchor role in the new hub. The company has more than three decades of experience making biologics, the fastest-growing class of drugs, which includes best-sellers like Herceptin, Remicade, Humira and Avastin. Biologics are proteins grown by genetically modified cells cultured in tanks called bioreactors. GE makes bioreactors as well as other technology required to produce these drugs. “In the biopharmaceutical industry, we use cells in bioreactors to make these therapeutic proteins,” GE’s Vanek says. “We can use similar technology to multiply reengineered cells for cell therapy. Just like cells producing proteins, cells for therapy have to be washed, multiplied, purified, concentrated and packaged. We already know how to do that. But unlike bioprocessing, where the cells are discarded and only the protein is saved, we collect intact living cells and this introduces added complexity to the process.”
Vanek has other tools in his kit. In many ways, GE Healthcare’s cell therapy business is the perfect example of what the company calls the GE Store — the ability to share knowledge across many domains. The team works with GE’s bioprocess business in Uppsala, the HyClone team in Cardiff, software engineers in Bangalore and San Ramone, scientists at GE Global Research and GE Ventures. They will be also using Predix, the cloud-based software platform for the Industrial Internet developed by GE Digital. “Our fate is determined by these collaborations,” Vanek says.
For example, cellular immunotherapy starts with the patient’s own cells. Vanek says Predix could allow manufacturers to keep a digital chain of custody of those cells. “We call it the digital thread and already use it in manufacturing,” he says. “It could allow us to track cells through the whole reprogramming and manufacturing process. We could run real-time analytics during the process and then ultimately follow the patient results. Since every patient introduces a level of biological variability, we envision smart systems in the future that could adapt the production process in real-time depending on the biology that’s coming in.”
Last year GE launched the GE Health Cloud, which allows hospitals to collect and work with patient data. Vanek says that, to be broadly adopted, cell therapy manufacturing processes will have to be flexible, push-button, sterile and disposable.
The new center will help, says CCRM’s May. He believes that better-designed cell therapy tool kits for clinical production could be available within a few years, and “manufacturing blueprints” by the end of the decade. Says May: “The new investment will help us break through the manufacturing bottlenecks and get us there.”





