The treatment would be taxing. She would need to either undergo surgery to remove part of her liver or be treated by rounds of chemotherapy or radiation, or both. And the prognosis was bleak — even with this aggressive strategy, she would potentially have only a few more months to live.
For Jansson, who had spent the past few years battling myriad health challenges, those extra months just weren’t worth the treatment’s physical toll. “I have had too many family members who went through chemo and radiation,” Jansson explained. “When I found out that this option would only buy me a few months, I decided to ride it out and, if it was my time, to die.”
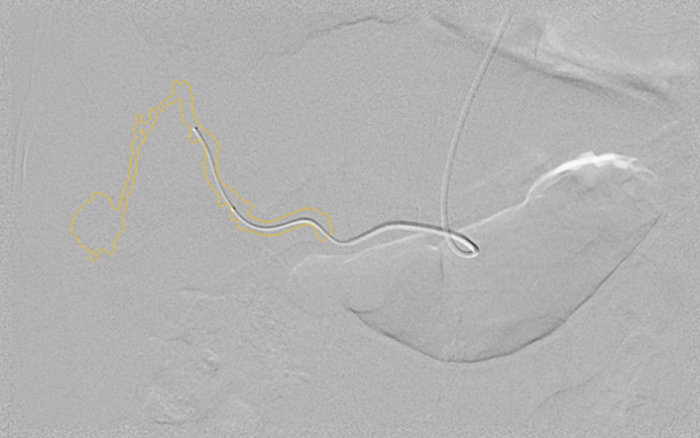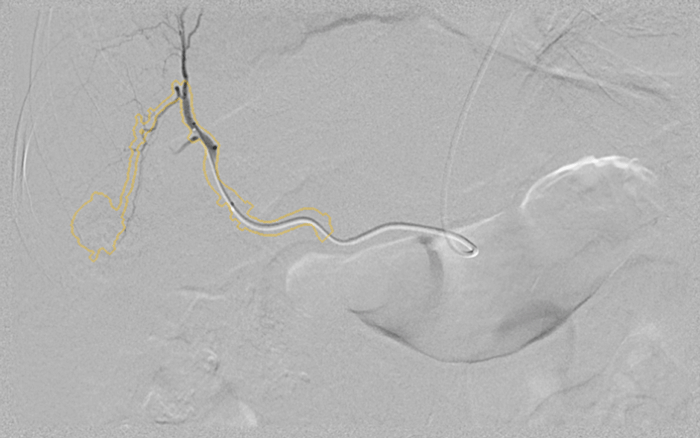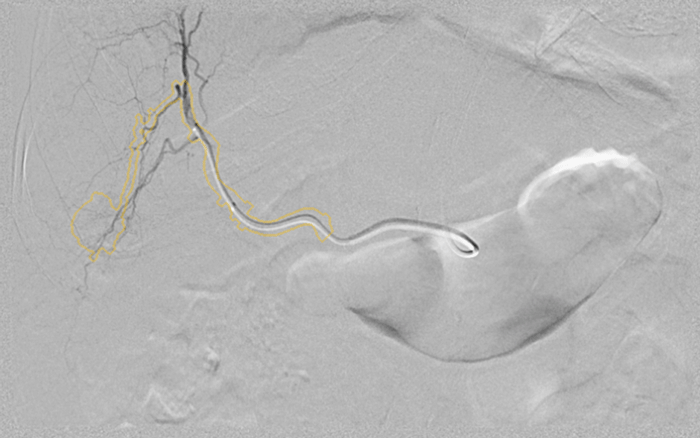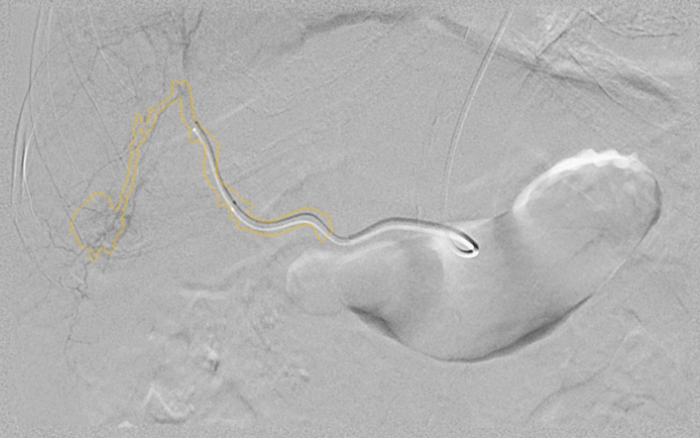
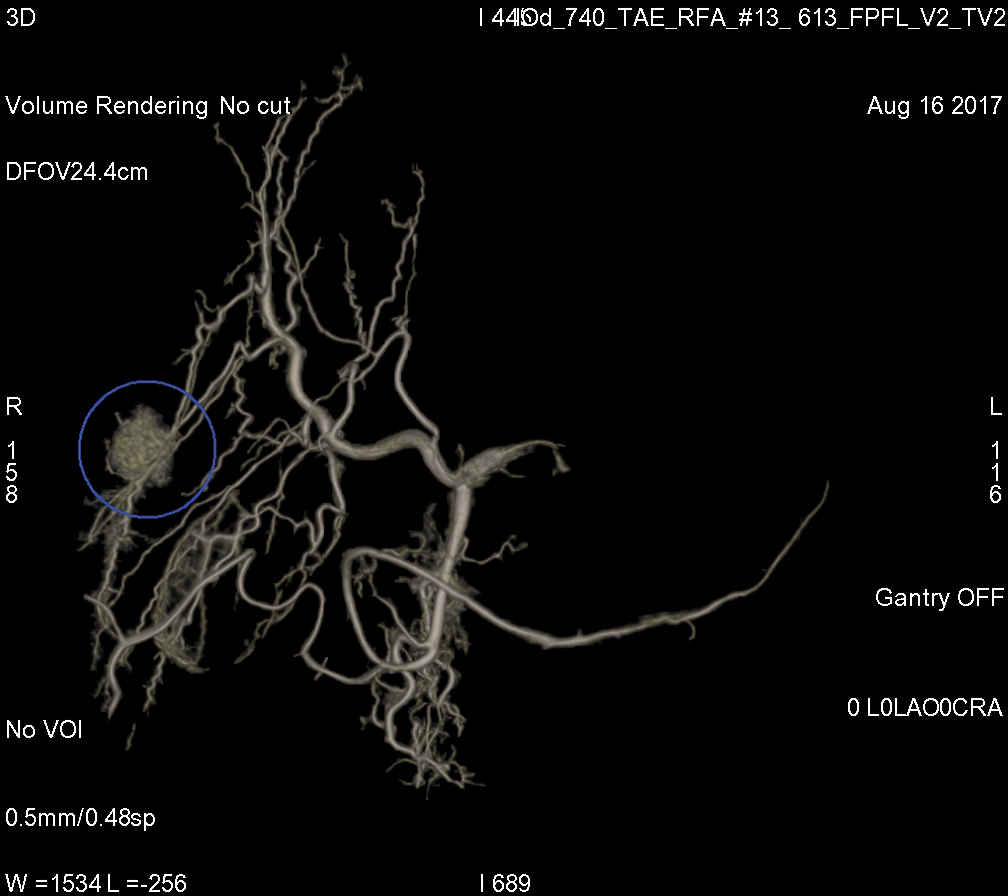 When Georgeann Jansson was diagnosed with liver cancer, her doctor recommended a minimally invasive treatment called transarterial chemoembolization (TACE). The approach uses a catheter guided by an X-ray scanner to deliver chemotherapy and other materials to the liver. Images credit: GE Healthcare.
When Georgeann Jansson was diagnosed with liver cancer, her doctor recommended a minimally invasive treatment called transarterial chemoembolization (TACE). The approach uses a catheter guided by an X-ray scanner to deliver chemotherapy and other materials to the liver. Images credit: GE Healthcare. But then an acquaintance told her about Dr. Marcelo Guimaraes, a vascular interventional radiologist at the Medical University of South Carolina (MUSC) who has successfully treated patients with cancer in a less invasive way. So she sought out a second opinion.
Jansson met with Guimaraes, who recommended a procedure called transarterial chemoembolization (TACE). This minimally invasive approach uses a catheter guided by an X-ray scanner to deliver local chemotherapy, Lipiodol — a poppy-seed oil that is opaque to radiation — and special beads to block blood vessels in the liver. Because the chemotherapy is precisely targeted and the Lipiodol and beads help reduce the amount of medicine leaving the liver, patients typically do not suffer traditional chemotherapy’s side effects.
Guimaraes suggested pairing TACE with radiofrequency ablation therapy, which uses a heating probe to kill tumors. After a long discussion, Jansson agreed to the procedure. “No radiation, no chemo, in and out of the hospital — it sounded like parole to a prisoner!” Jansson said. “I was totally floored by Guimaraes’s knowledge and dedication to the procedure.”
Days later, Jansson arrived at MUSC. Guimaraes placed her in the angiography suite, made a 2-millimeter incision in her arm and used the GE Discovery IGS 740 imaging system to take 3D scans to locate the artery supplying the tumor with blood. He then used a different GE technology called Liver ASSIST to help pinpoint where to maneuver the catheter and release the mix of Lipiodol chemotherapy followed by beads.
Once the beads were injected, Guimaraes used the imaging solutions to help him determine the needle trajectories for radiofrequency ablation. Then he inserted the needles around the tumor and applied heat to reduce its size.
The entire procedure took three hours, and Jansson was released from the hospital that day. Within a week, she completely recovered from any surgery site pain, and one month later she received a follow-up MRI, which showed promising results: The tumor was dead, without evidence of residual disease or complication.
Today, over a year since Jansson’s initial appointment with Guimaraes, her tumor remains under control, with no signs of recurrence or new lesions. While Guimaraes will continue to regularly monitor her liver, Jansson feels incredibly relieved.
“Every day is a gift,” she said. “Even though I have other diseases to contend with, it’s the mental freedom from this that makes me feel better. I’m here and able to see a new day, and that is directly due to Guimaraes and his staff, their knowledge and dedication and the technology that kept me here.”
A version of this article originally appeared on The Pulse, GE Healthcare’s newsroom.