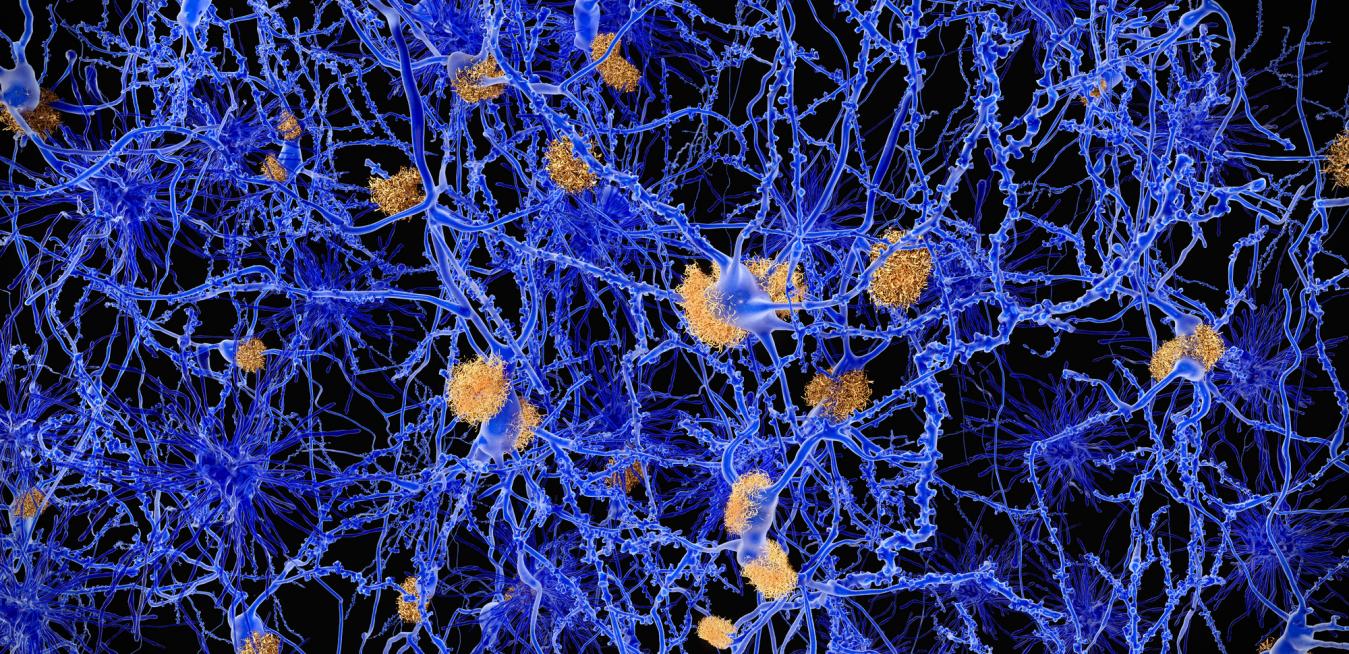
A team at the Karolinska Institute watched brain cells called astrocytes, which protect and support the information-carrying neurons, increase in number years before people genetically predisposed to the disease showed any symptoms. Researchers believe this phenomenon is the body's inflammatory response to the earliest stages of Alzheimer's, a form of dementia in which protein fragments called amyloid clump together in plaques that damage brain tissue.
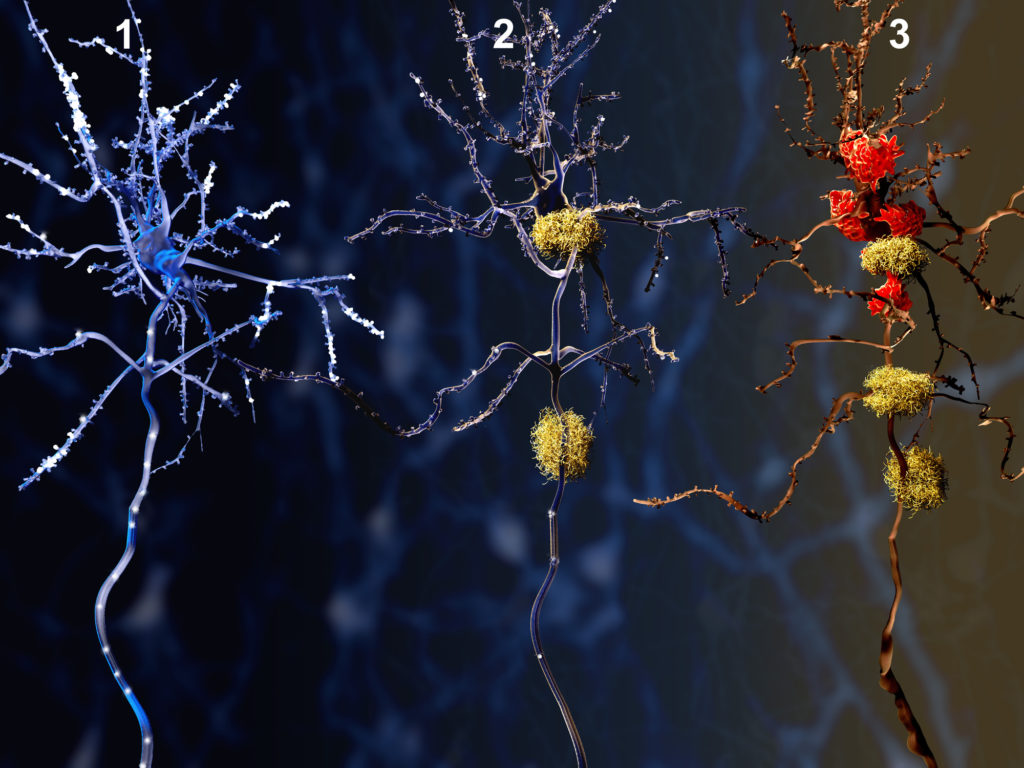 Top image and above: These illustrations show neurons with amyloid plaques. Above: 1. Healthy neuron. 2. Neuron with amyloid plaques (yellow). 3. Dead neuron being digested by microglia cells (red) Images credit: Getty Images
Top image and above: These illustrations show neurons with amyloid plaques. Above: 1. Healthy neuron. 2. Neuron with amyloid plaques (yellow). 3. Dead neuron being digested by microglia cells (red) Images credit: Getty Images“Astrocytes are like soldiers — they see amyloid appear and they try to stop it,” says Agneta Nordberg, a medical doctor and neuroscientist at the institute. “That's why we think the increase in astrocytes could be an indicator that pathological change is starting in the brain. They're trying to remove the proteins, but amyloid accumulation is too strong for them.”
Since 2010, GE Healthcare has been supporting the research with a multiyear grant totaling some 400,000 euros.
Getting more insight into Alzheimer's is critical for the growing number of people around the world who suffer from the progressively debilitating brain disease, which robs patients of their memories and the ability to perform even the most basic tasks. Last year, 5 million Americans and 47 million people worldwide were afflicted with it, and that number is projected to increase to 75 million globally by 2030.
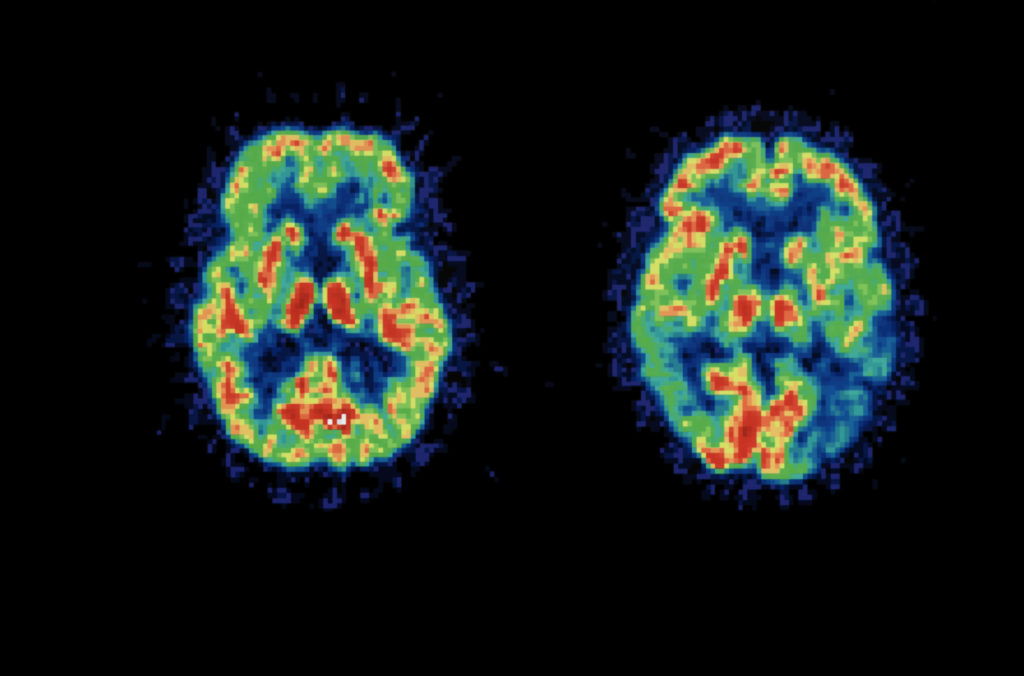 Brain scan comparison. Left brain shows reduced activity. Image credit: Getty images
Brain scan comparison. Left brain shows reduced activity. Image credit: Getty imagesTo uncover astrocytes' previously hidden role, the team studied 52 people with mutations known to significantly increase the risk of acquiring Alzheimer's. All of the participants underwent memory tests. They were then injected with radioactive tracers that highlight different features in the brain and scanned with a positron emission tomography (PET) machine. Half of the subjects were scanned again three years later so the team could identify brain changes over that time.
Putting that data into computer models, Nordberg and her colleagues saw an unexpected relationship. They observed the first deposits of a type of protein fragment called amyloid-β occurring some 17 years before the expected onset of symptoms.
At the same time, the number of astrocytes in the brain began increasing. Interestingly, the number of astrocytes spiked as amyloid began accumulating and then declined while plaque deposition increased over time. “Astrocyte activation peaks roughly 20 years before the expected symptoms and then goes into decline, in contrast to the accumulation of amyloid plaques, which increases constantly over time until clinical symptoms show,” Nordberg says. “The accumulation of amyloid plaque and the increase in number of astrocytes therefore display opposing patterns along the timeline.”
The work was revealed in papers published last year and in late January in the journals Nature Scientific Reports and Brain. The finding means that astrocytes could become a very early diagnostic marker of Alzheimer's. Research in the cells could lead to new treatments for the disease.
The disorder is also associated with structural molecules called tau proteins, which normally help keep vital nutrients and other products flowing to neurons but can get tangled up and block proper cell functioning. Nordberg says the next steps for research should focus on how tau proteins relate to the astrocyte-amyloid relationship.
“To treat Alzheimer's disease, we must first understand the course of its progression over time and develop diagnostic markers to detect it,” she says. “This line of research offers a new way to understand it, and it also raises the question, can we use this knowledge to develop new therapies?”