Machine learning is helping researchers develop potential COVID-19 vaccines, the world’s fastest computer shed some light into the coronavirus’ strange effects on the body, and a new discovery could lead to electric-vehicle batteries that recharge more efficiently. Also in this week’s coolest scientific findings: a smart thermometer that can take the temperatures of up to nine people at once.
What is it? A team from the Massachusetts Institute of Technology’s Computer Science and Artificial Intelligence Laboratory, or CSAIL, designed a machine learning system to predict how well a COVID-19 vaccine might work among broad populations of people.
Why does it matter? OptiVax, as the system is called, “introduces methods for designing new peptide vaccines, evaluating existing vaccines, and augmenting existing vaccine designs,” according to MIT News. It’s described in a new article in Cell Systems.
How does it work? The technology revolves around peptides — short strings of amino acids that, in the case of the coronavirus, help the virus infect humans by attaching to cell surfaces. Because vaccines use parts of the virus to train the immune system to recognize and fight it, researchers involved in the development of COVID-19 peptide vaccines are looking for “which peptides will fit in the groove of surface cell receptors,” according to ZDNet’s Tiernan Ray, who calls this “a matching problem on a large scale.” That’s where machine learning comes in: It was able to quickly search through about 155,000 peptides and model which ones would best combine with surface cell receptors. OptiVax also takes into account the genetic makeup of different human populations in order to maximize the number of people whom a vaccine might be effective on.

What is it? Speaking of COVID-19 and computers: Researchers at Oak Ridge National Laboratory (ORNL) used Summit, the world’s fastest supercomputer, to analyze the lung fluid of infected patients in hopes of shedding light into “the runaway symptoms produced by the body’s response to SARS-CoV-2,” the coronavirus that causes COVID-19.
Why does it matter? COVID-19 is notorious for its effects on the respiratory system, but many patients have suffered a bewildering array of symptoms all over the body: muscle pain, impaired cognitive function, nausea and diarrhea. In hopes of understanding the manifold complications COVID-19 can produce, the ORNL team analyzed genes from cells in the lung fluid from nine infected patients, comparing the results to 40 control patients. The use of the supercomputer meant results in a week, rather than the months the calculations would’ve taken on a regular desktop computer.
How does it work? In an article in eLife, ORNL’s Dan Jacobson and his colleagues propose that bradykinin — part of a body system responsible for lowering blood pressure — is “overproduced” in COVID-19 patients, leading to leaky blood vessels and allowing fluid to build up in the soft tissues. A “bradykinin storm,” according to ORNL, could “explain the wide variety of symptoms experienced by COVID-19 patients.” If supported by further study, these findings could offer new ideas into how to treat COVID-19 patients.
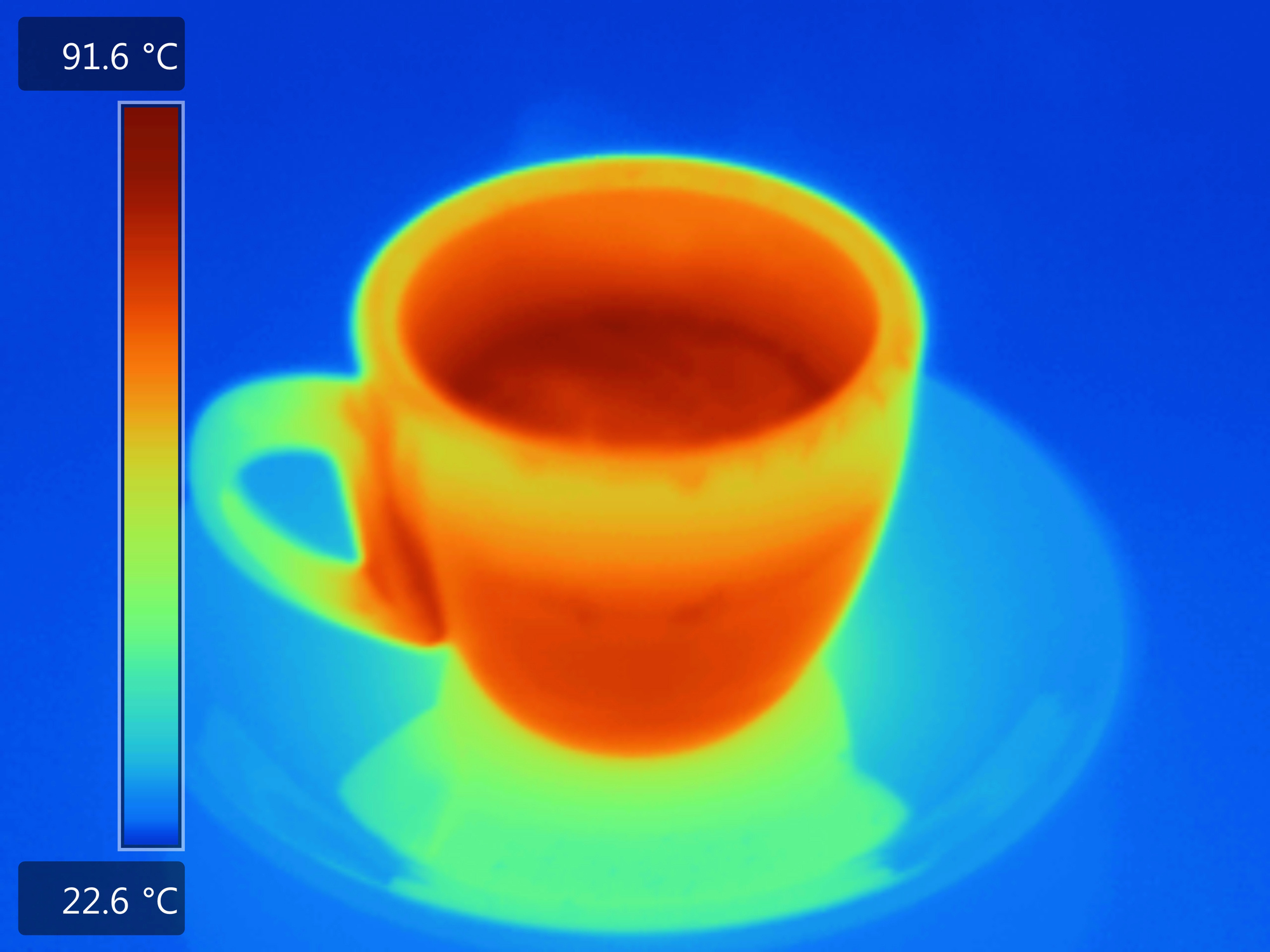
What is it? A team of researchers in Thailand has created a screening system that can take the temperatures of up to nine people at a time, whether or not they’re wearing face masks.
Why does it matter? Since fever is a symptom of COVID-19 infection, temperature checks are one way to screen people in public places, like airports or stores. The new device combines a visible camera, a thermal imaging camera, lidar and facial recognition technology with an algorithm that compensates for distance shift, which “occurs when several individuals being checked are not at the same measuring distance, leading to a fluctuation in temperature measurements,” according to IEEE Spectrum, which interviewed one of the creators of the system, Sarun Sumriddetchkajorn.
How does it work? Sumriddetchkajorn explains that the system, called µTherm-FaceSense, “basically looks for all faces in its field of view, and then simultaneously analyzes the corresponding facial temperatures [of each]. If the temperature of any person detected is equal to or above the threshold value, for example, 37.5° C, his or her temperature value is highlighted in red on a display screen and a beep sounds.”

What is it? Materials scientists studying the fundamentals of lithium recharging “made an astonishing discovery that could open the door to better batteries, faster catalysts and other materials science leaps,” according to a news release from the University of California San Diego, whose scientists were responsible for the findings alongside colleagues from Idaho National Laboratory.
Why does it matter? The research was funded by the Department of Energy’s Battery500 initiative, which is challenging scientists to develop commercially viable batteries for electric vehicles that can deliver 500 watt-hours per kilogram — with the ultimate vision of smaller, lightweight, more affordable batteries and therefore more affordable electric cars. The findings are described at length in Nature Materials.
How does it work? Lithium is a preferred material in rechargeable batteries, but the recharging process at the atomic level remains poorly understood, and can result in reduced battery life and erratic charging. Never before observed, the new material — described as “glassy lithium” — springs from researchers’ observation that “slow, low-energy charging causes electrodes to collect atoms in a disorganized way that improves charging behaviors,” per UC San Diego. The new understanding underlying the material could also lead to “more effective metal catalysts, stronger metal coatings and other applications that could benefit from glassy metals.”
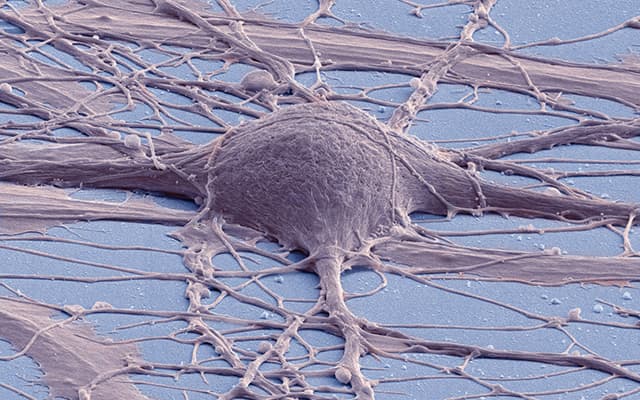
What is it? Also at UC San Diego — specifically the School of Medicine — scientists successfully implanted neural stem cell grafts into mice with spinal cord injuries and were able to monitor how the grafts grew to fill the injury sites.
Why does it matter? Using stem cells to restore function to people with spinal cord injuries has “long been an ambition of scientists and doctors,” according to the medical school, and while previous attempts to graft stem cells onto spinal cord injuries in mice had shown results, it was hard for scientists to see exactly what was going on — the process was a “black box.”
How does it work? Using light rather than electricity to both stimulate and record the activity of neurons, the researchers were able to observe both host and graft neurons and their interplay. “We showed that we could turn on spinal cord neurons below the injury site by stimulating graft axons extending into these areas,” Steven Ceto, lead author of a paper in Cell Stem Cell, said. “Putting all these results together, it turns out that neural stem cell grafts have a remarkable ability to self-assemble into spinal cord-like neural networks that functionally integrate with the host nervous system.”





